KEY TAKEAWAY:
--The technology has the potential to lower claims costs by up to $1,000 per claim and eliminate the historical delay in the traditional accident reporting process, which averages five days from accident to first notice of loss.
-----------
Too many headlines contain wild hyperbole meant to grab readers’ attention while conveying the enthusiasm of the author. In particular, the word “transformation” has been severely overused and often misplaced, particularly when applied to the auto insurance claims process. This is NOT the case here!
It is our opinion, as experts in auto physical damage claims information technology, that the more sophisticated crash detection as defined here will indeed be transformative to auto claims in multiple ways.
But first it is critical to understand the relationships among various telematics programs and crash detection technologies.
Telematics: A Brief History
Telematics, in one iteration or another, has been around since GM introduced its OnStar in-vehicle telematics technology and related safety services. OnStar was initially a dealer-installed device offered in several 1997 Cadillac models. OnStar enabled drivers to connect from their cars with safety advisers in the event of an accident, breakdown or other roadside emergency.
Since then, the convergence of telecommunications and information processing – broadly referred to as telematics – enabled the use of information such as vehicle location, driver behavior, engine performance and vehicle activity. Numerous telematics service providers (TSPs) emerged globally to offer a wide variety of uses across a number of market verticals. In 2002, Octo Telematics was founded in Italy specifically for use cases in the auto insurance industry, originally including fraud, theft and location services.
These early applications required the installation of some type of in-vehicle hardware device (dongles, sensors, windshield tags, etc.). TSP solutions included commercial applications for fleet management, as well as personal lines auto insurance applications including usage-based insurance (UBI) and pay-as-you-drive (PAYD).
In 2015, a smartphone app-based driver behavior tech company was spun out of Harvard Innovation Labs. Censio was renamed True Motion and was acquired by Cambridge Mobile Telematics (CMT) in 2021. The company’s mission was safer and more affordable driving. CMT has grown to become the world leader in telematics and powers many of the largest insurance telematics programs in the U.S. and globally.
Consumer adoption within the auto insurance landscape still remains in the low double digits but continues to gain traction as loss costs and premiums continue to rise and consumers seek savings options. Adoption in North America has lagged other global markets for a variety of regulatory and cultural reasons.
More recently, a specific application of telematics – namely crash detection – has emerged as new model smartphones include high-dynamic-range gyroscopes, GPS location, barometers, microphones and advanced motion algorithms that can detect a crash.
See also: How to Reduce Distracted Driving
Accident Detection and False Positives
With the introduction of smartphone accident detection in 2015 by Zendrive, a driver-centric analytics company, variations of crash detection began to emerge, mostly for notifying emergency services, tow trucks and family members. Other applications included the gathering of accident- related data for future use in insurance claims.
Most recently, there have been a number of stories about new model smartphones and connected devices with crash detection features alerting early responders to crashes – both real and not.
But beyond these kinds of crash detection, another application is emerging for use specifically in auto insurance accident claims that has the potential to truly transform this process by lowering claims costs by up to $1,000 per claim and eliminating the historical delay in the traditional accident reporting process, which averages five days from accident to first notice of loss.
Crash Detection and the Auto Insurance Claims Process
Before any insurer would consider deploying a crash detection program, there are two critical technical issues to be overcome: namely, accuracy in detecting real accidents (at speeds below 25 mph) and the elimination of “false positives,” in which sensors misinterpret motion as accidents when it may be something as simple as an accidentally dropped phone, energetic dancing at the Bonnaroo festival or a wild ride on a roller coaster.
No carrier would want to waste valuable resources and risk annoying their policyholders by contacting them unnecessarily when no accident has occurred. On the other hand, all carriers would find it valuable to be alerted to real crashes in real time. In addition, documented crash details would have great value.
Right on cue just last month, Sfara, a global telematics technology provider that launched the first mobile phone-based crash detection in 2014, introduced capabilities that solve both of the technical issues.
The distinction between basic crash detection and all-speed, false-positive-free crash detection is critical for effective deployment in an auto insurance claims application.
Low-speed accident detection for claims is more valuable than many may think. Sfara research finds that 70% of crashes occur under 25 mph, as do 48% of crashes involving injuries--and solutions that only capture high-speed accidents miss all of them. 11% of fatalities occur when a vehicle is not moving at all.
Sfara Crash Detection
Sfara has formed strategic partnerships with Mercedes Benz; Bosch; CCC Intelligent Solutions, the industry’s leading auto insurance physical damage information provider; and Solera eDriving, a global digital driver risk management provider for fleets. These relationships enable insurance companies and fleets that are already integrated with these companies’ solutions to operationalize Sfara’s crash detection results quickly and easily through the simple addition of the Sfara SDK to their flagship smartphone apps. Several top 10 carriers have already begun. Thus, real crash detection becomes available to all policyholders, not just the minority who are enrolled in telematics programs.
See also: Could Auto Accidents Be Reduced by More Than Half?
Insurer Adoption
Crash detection, and its first cousin accident response, are poised to see real traction with auto insurers.
In September, State Farm joined USAA, which incorporated crash detection capabilities into their respective mobile applications a year earlier. In February, Progressive Insurance announced the planned introduction of their app-based accident response service to offer towing and emergency services and to start a claim after an accident.
Importantly, however, none of these programs have indicated that they can offer service at all speeds.
The Future
Real crash detection, such as that offered by Sfara, is poised for rapid adoption by auto insurers and will literally transform the auto insurance claims process, including first notice of loss (FNOL), which has historically occurred many days after an accident and been labor-intense. Crash detection will enable digital FNOL in real time and can include accident management, triage of roadside services, automated scheduling of vehicle repairs, photo estimating, parts ordering and other use cases not yet envisioned. And because it is low- to no-touch and technology-powered, its cost to carriers will be nominal.
Crash detection is perfectly aligned with emerging claims process digitization initiatives and will significantly reduce loss costs, thus materially improving combined ratios. It is also well-aligned with the industry’s strategic shift underway in claims strategy from a "repair and replace" to a "predict and prevent" mindset: Crash detection can be the portal through which future advances in vehicle and driver safety can be delivered.
Real-time crash detection and FNOL will help transform the traditional mindset in claims operations to focus on speed of resolution. Equally valuable is the crash data captured with detection, which is instrumental in the claim investigation process. Think of crash detection as an unbiased “witness” gathering all the critical information on speed, direction of travel, point of impact and more.
Auto insurance financial performance is under extreme pressure as costs continue to rise, as vehicle complexity increases, as the workforce is aging out and taking critical expertise with them and as unsustainable, higher insurance premiums are meeting resistance from regulators. Crash detection can deliver significant relief quickly and at low cost.
Policyholders will embrace crash detection once they understand that it is all upside and no downside. Emergency services and accident response will be especially welcome, as will the elimination of irritating phone calls that require repeating accident details to multiple agents. Claims resolution and cycle times, including the return of repaired vehicles, will be materially improved.
Auto insurance ecosystem partners will see operational benefits and savings through increased real-time, digitally integrated workflow and the elimination of legacy communications and labor intense processes.
See also: Auto Insurance in an Existential Crisis
Call to Action
With the arrival of true crash detection, auto insurers should learn, test, pilot and implement this technology as one of their highest priorities. Their stakeholders and partners will be most appreciative, and their customers will reward them with greater loyalty.
Crash detection will transform auto claims and become table stakes, and it will be no accident – which is definitely not hyperbole.









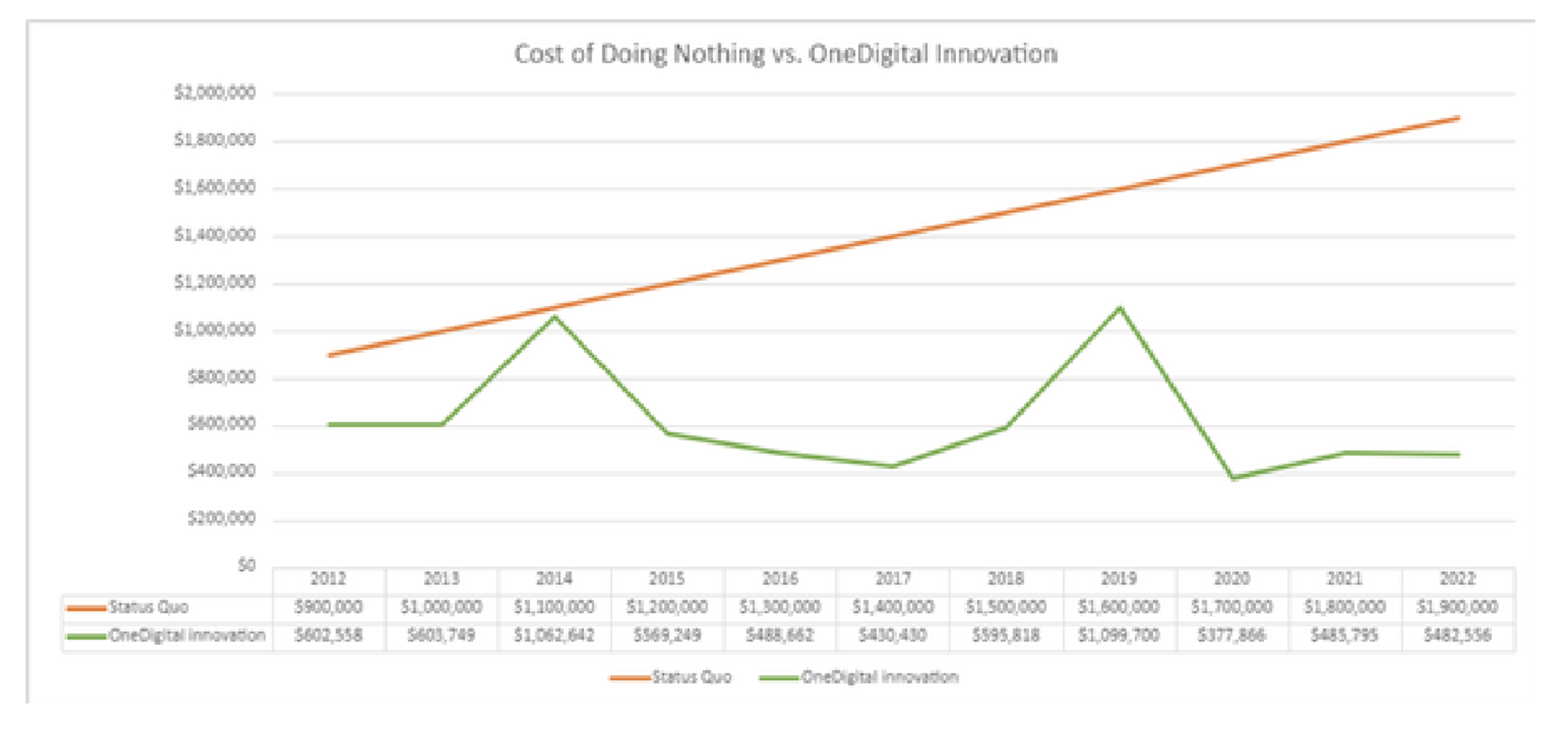 Employers with a substantial payroll, a strong commitment to workplace safety and a desire to reduce workers' compensation expenses should consider this option.
Employers with a substantial payroll, a strong commitment to workplace safety and a desire to reduce workers' compensation expenses should consider this option.