Educating Smokers: the Best Insurance
Insurance agents have it within their power to do more than sell policies or find the best prices for smokers who want to buy insurance.

Insurance agents have it within their power to do more than sell policies or find the best prices for smokers who want to buy insurance.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|
In 2012-17, P&C industry loss ratios improved by 18 points, while 20 carriers that used predictive analytics well gained 35 points.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Kirstin Marr is the executive vice president of data solutions at Insurity, a leading provider of cloud-based solutions and data analytics for the world’s largest insurers, brokers and MGAs.
The study that said no level of drinking of alcohol is safe suffers from the same flaws in statistical analysis that afflict so many wellness studies.

 Or NPR:
Or NPR:
 And how often do those two outlets agree with Fox News?
And how often do those two outlets agree with Fox News?
 One thing you learn if you hang around wellness promoters long enough is that oftentimes a close perusal of the study in question shows the opposite of what the authors intended. Or, as we often say: “In wellness, you don’t have to challenge the data to invalidate it. You merely have to read the data. It will invalidate itself.” And the same is true here.
For example, Denmark leads the world in the number of drinkers — and has life expectancy higher than about 90% of the world’s countries. The lowest alcohol consumers? Pakistan — which ranks #130 in life expectancy. You might say: “Wait, aren’t there many other factors involved in life expectancy?” And the answer is, of course there are. None of those were controlled for in any way in this meta-analysis. To begin with, the more people drink, the more other unhealthy habits they are likely to have.
But that’s not the crux of what is wrong with this study. Two other things should lead wellness professionals to the opposite conclusion: that light drinking is perfectly OK. The remainder of this post addresses those.
Absolute risk vs. relative risk
Absolute vs. relative risk is one of our (many) pet peeves. Here are two other examples that we have had to smack down:
One thing you learn if you hang around wellness promoters long enough is that oftentimes a close perusal of the study in question shows the opposite of what the authors intended. Or, as we often say: “In wellness, you don’t have to challenge the data to invalidate it. You merely have to read the data. It will invalidate itself.” And the same is true here.
For example, Denmark leads the world in the number of drinkers — and has life expectancy higher than about 90% of the world’s countries. The lowest alcohol consumers? Pakistan — which ranks #130 in life expectancy. You might say: “Wait, aren’t there many other factors involved in life expectancy?” And the answer is, of course there are. None of those were controlled for in any way in this meta-analysis. To begin with, the more people drink, the more other unhealthy habits they are likely to have.
But that’s not the crux of what is wrong with this study. Two other things should lead wellness professionals to the opposite conclusion: that light drinking is perfectly OK. The remainder of this post addresses those.
Absolute risk vs. relative risk
Absolute vs. relative risk is one of our (many) pet peeves. Here are two other examples that we have had to smack down:
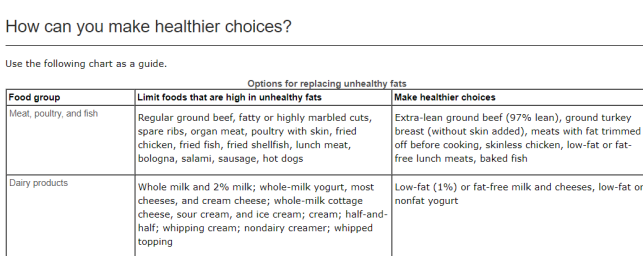 Here is Optum railing against oils:
Here is Optum railing against oils:
 And Cerner, once again, this time incriminating dietary cholesterol, which of course has no impact on blood cholesterol for most people:
And Cerner, once again, this time incriminating dietary cholesterol, which of course has no impact on blood cholesterol for most people:
 Finally, here is Interactive Health hyperventilating about something-or-other in its HRA feedback to an employee. We don’t know what it is other than, given the provenance, it’s wrong. Fortunately, no employee is going to plow through this anyway.
Finally, here is Interactive Health hyperventilating about something-or-other in its HRA feedback to an employee. We don’t know what it is other than, given the provenance, it’s wrong. Fortunately, no employee is going to plow through this anyway.
 Conclusion
Treat this alcohol finding the same way you would treat advice from most health risk assessments: ignore it.
Conclusion
Treat this alcohol finding the same way you would treat advice from most health risk assessments: ignore it.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Al Lewis, widely credited with having invented disease management, is co-founder and CEO of Quizzify, the leading employee health literacy vendor. He was founding president of the Care Continuum Alliance and is president of the Disease Management Purchasing Consortium.
A hundred thousand homeowners who were told they did not need flood insurance had their homes severely damaged by Harvey.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Albert J. Slap is president and co-founder of Coastal Risk Consulting, the first company to provide millions of coastal homeowners in the U.S., as well as businesses and local governments, with online, state-of-the-art, climate risk assessments at an affordable price.
Gone are the days of 24- to 36-month IT projects. Insurers need to act now and act fast to deliver new products.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Brian Harrigan, CEO of InsurIQ, a provider of insurance technology solutions, has spent over 40 years in the insurance industry, helping agents and carriers manage the purchasing of insurance and personal protection products.
Insurtech names could provide a whole meal (Oyster, Pineapple, Cake, Pie) or fill a zoo (Blue Zebra, Bold Penguin, Rhino, Hippo).

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Mark Breading is a partner at Strategy Meets Action, a Resource Pro company that helps insurers develop and validate their IT strategies and plans, better understand how their investments measure up in today's highly competitive environment and gain clarity on solution options and vendor selection.
There is one answer that keeps coming up to the question of "What makes an insurtech initiative a success?" That answer – the team.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Stephen Goldstein is a global insurance executive with more than 10 years of experience in insurance and financial services across the U.S., European and Asian markets in various roles including distribution, operations, audit, market entry and corporate strategy.
The lack of original copy from agents—the general absence of creativity—is a symptom of personal laziness and professional indifference.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|
When asked, “Why should I do business with you/your agency?” most will respond with the same standard, boring, "Generic Five" lines.

 What is one doing to get the prospect’s business that the other one isn’t? When an opportunity arrives, what are you/your producers doing and saying to connect with the prospect and close the deal? What’s your process, and how do you follow up on it?
What is one doing to get the prospect’s business that the other one isn’t? When an opportunity arrives, what are you/your producers doing and saying to connect with the prospect and close the deal? What’s your process, and how do you follow up on it?
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|
Yes, AI will change everything. But that doesn't mean the technology need be daunting, or that insurers lack the skills to tackle the challenge.

 Data: AI might be considered the key that unlocks the door of big data. Many of the modeling techniques that fall under the AI umbrella are classification algorithms that are data hungry. Unlocking the power of these methods requires sufficient volume of training data. Data takes several forms. First, there are third party data sources that are considered external to the insurance industry. Aerial imagery (and the processing thereof) to determine building characteristics or estimate post-catastrophe claims potential are easy examples. Same with the vast quantities of behavioral data built on the interactions of users with digital platforms like social media and web search. Closer to home, insurance has long been an industry of data, and carriers are presumed to have meaningful datasets in claims, applications and marketing, among others.
Infrastructure: Accessing the data to feed the AI requires a working infrastructure. How successfully can you ingest external data sources? How disparate and unstructured can those sources be? Cloud computing is not necessarily a prerequisite to successful AI, but access to vast, scalable infrastructure is enabling. Are your information systems equipped, including security vetting, to do modeling in the cloud? Can you extract your internal data into forms that are ready to be processed using advanced modeling techniques? Or are you running siloed legacy systems that prevent using your proprietary data in novel ways?
Talent: Add data science to the list of AI-related buzzwords. We claimed earlier that many of the advancements attributed to narrow AI are predictive models conceptually like modeling techniques already used in the insurance industry. However, the fact that your pricing actuary conceptually appreciates an artificial neural net built for fraud detection using behavioral data does not mean you have the in-house expertise to build such a model. Investments in recruiting, training and retaining the right talent will provide two clear benefits. The first benefit is being better equipped to do the risk-cost-benefit analysis of which data and methods to explore. The second is having the ability to test and, ultimately, implement.
See also: 4 Ways Connectivity Is Revolutionary
In Aon’s 2017 Global Insurance Market Outlook we explored the idea of the third wave of innovation as propounded by Steve Case, founder of AOL, in his book, “The Third Wave: An Entrepreneur’s Vision of the Future.” The upshot of the third wave for insurers was that partnership with technology innovators, rather than disruption by them, would be the norm. This approach applies now more than ever as technological innovators continue to unlock the potential of AI. If you don’t have the data, or the infrastructure, or the talent to bring the newest technologies to bear, you can partner with someone that does. Artificial intelligence is real. While the definitions are somewhat vague - is it software, predictive models, neural nets or machine learning - and the hype can be difficult to look past, the impacts are already being felt in the form of chatbots, image processing and behavioral prediction algorithms, among many others. The carriers that can best take advantage of the opportunities will be those that have a pragmatic ability to evaluate tangible AI solutions that are incremental to existing parts of their value chain.
“If you don’t have an AI strategy, you are going to die in the world that’s coming.” Devin Wenig CEO, eBay
Maybe true, but that does not make it daunting. The core of insurance is this: Hire the right people, give them the infrastructure they need to evaluate risk better than the competition and curate the necessary data to feed the classification models they build. AI hasn’t, and won’t, change that.
Data: AI might be considered the key that unlocks the door of big data. Many of the modeling techniques that fall under the AI umbrella are classification algorithms that are data hungry. Unlocking the power of these methods requires sufficient volume of training data. Data takes several forms. First, there are third party data sources that are considered external to the insurance industry. Aerial imagery (and the processing thereof) to determine building characteristics or estimate post-catastrophe claims potential are easy examples. Same with the vast quantities of behavioral data built on the interactions of users with digital platforms like social media and web search. Closer to home, insurance has long been an industry of data, and carriers are presumed to have meaningful datasets in claims, applications and marketing, among others.
Infrastructure: Accessing the data to feed the AI requires a working infrastructure. How successfully can you ingest external data sources? How disparate and unstructured can those sources be? Cloud computing is not necessarily a prerequisite to successful AI, but access to vast, scalable infrastructure is enabling. Are your information systems equipped, including security vetting, to do modeling in the cloud? Can you extract your internal data into forms that are ready to be processed using advanced modeling techniques? Or are you running siloed legacy systems that prevent using your proprietary data in novel ways?
Talent: Add data science to the list of AI-related buzzwords. We claimed earlier that many of the advancements attributed to narrow AI are predictive models conceptually like modeling techniques already used in the insurance industry. However, the fact that your pricing actuary conceptually appreciates an artificial neural net built for fraud detection using behavioral data does not mean you have the in-house expertise to build such a model. Investments in recruiting, training and retaining the right talent will provide two clear benefits. The first benefit is being better equipped to do the risk-cost-benefit analysis of which data and methods to explore. The second is having the ability to test and, ultimately, implement.
See also: 4 Ways Connectivity Is Revolutionary
In Aon’s 2017 Global Insurance Market Outlook we explored the idea of the third wave of innovation as propounded by Steve Case, founder of AOL, in his book, “The Third Wave: An Entrepreneur’s Vision of the Future.” The upshot of the third wave for insurers was that partnership with technology innovators, rather than disruption by them, would be the norm. This approach applies now more than ever as technological innovators continue to unlock the potential of AI. If you don’t have the data, or the infrastructure, or the talent to bring the newest technologies to bear, you can partner with someone that does. Artificial intelligence is real. While the definitions are somewhat vague - is it software, predictive models, neural nets or machine learning - and the hype can be difficult to look past, the impacts are already being felt in the form of chatbots, image processing and behavioral prediction algorithms, among many others. The carriers that can best take advantage of the opportunities will be those that have a pragmatic ability to evaluate tangible AI solutions that are incremental to existing parts of their value chain.
“If you don’t have an AI strategy, you are going to die in the world that’s coming.” Devin Wenig CEO, eBay
Maybe true, but that does not make it daunting. The core of insurance is this: Hire the right people, give them the infrastructure they need to evaluate risk better than the competition and curate the necessary data to feed the classification models they build. AI hasn’t, and won’t, change that.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|