4 Goals for the NFL's Medical Officer
The NFL has the opportunity to be a national leader, ensuring that safety in healthcare comes first in America, on and off the field.

The NFL has the opportunity to be a national leader, ensuring that safety in healthcare comes first in America, on and off the field.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Leah Binder is president and CEO of <a href="http://www.leapfroggroup.org">the Leapfrog Group</a> (Leapfrog), a national organization based in Washington, DC, representing employer purchasers of healthcare. Under her leadership, Leapfrog launched the <a href="http://www.hospitalsafetyscore.org/">Hospital Safety Score</a>, which assigns letter grades assessing the safety of general hospitals across the country.
Insurers generally say their biggest enterprise risk comes from underwriting, but a quick test will usually show them they are wrong.

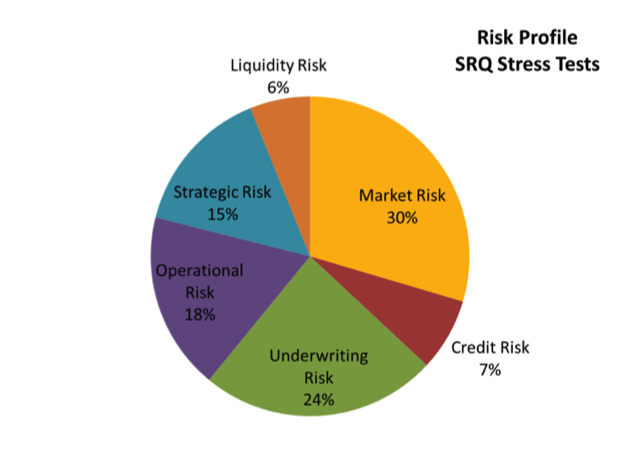 Stress tests are a good way for insurers to get started with looking at their risk profile. The six AM Best categories can be used to allow for comparisons with studies, or the company can use its own categories to make the risk profile line up with the main concerns of its strategic planning discussions. Be careful. Make sure that you check the results from the AM Best SRQ stress tests to make sure that you are not ignoring any major risks. To be fully effective, the risk profile needs to include all of the company’s risks. For 20 of these 31 insurers, that may mean acknowledging that they have more equity risk than underwriting risk – and planning accordingly.
Risk Profile From the BCAR Formula
The chart below portrays the risk profiles of a different group of 12 insurers. These risk profiles were determined using the AM Best BCAR formula without analyst adjustments. For this group of companies on this basis, premium risk is the largest single category. And while there are again six risk categories, they are a somewhat different list. The risk category of underwriting from the SRQ is here split into three categories of premium, reserve and nat cat. Together, those three categories represent more than 60% of the risk profile of this group of insurers. Operational, liquidity and strategic risks that make up 39% of the SRQ average risk profile are missing here. Reinsurer credit risk is shown here to be a major risk category, with 17% of the risk. Combined investment and reinsurer credit is only 7% of total risk in the SRQ risk profile.
Stress tests are a good way for insurers to get started with looking at their risk profile. The six AM Best categories can be used to allow for comparisons with studies, or the company can use its own categories to make the risk profile line up with the main concerns of its strategic planning discussions. Be careful. Make sure that you check the results from the AM Best SRQ stress tests to make sure that you are not ignoring any major risks. To be fully effective, the risk profile needs to include all of the company’s risks. For 20 of these 31 insurers, that may mean acknowledging that they have more equity risk than underwriting risk – and planning accordingly.
Risk Profile From the BCAR Formula
The chart below portrays the risk profiles of a different group of 12 insurers. These risk profiles were determined using the AM Best BCAR formula without analyst adjustments. For this group of companies on this basis, premium risk is the largest single category. And while there are again six risk categories, they are a somewhat different list. The risk category of underwriting from the SRQ is here split into three categories of premium, reserve and nat cat. Together, those three categories represent more than 60% of the risk profile of this group of insurers. Operational, liquidity and strategic risks that make up 39% of the SRQ average risk profile are missing here. Reinsurer credit risk is shown here to be a major risk category, with 17% of the risk. Combined investment and reinsurer credit is only 7% of total risk in the SRQ risk profile.
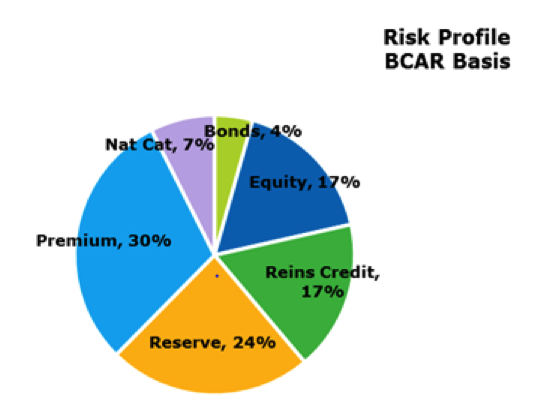 Why are the two risk profiles so different in their views about insurance and investment risks? This author would guess that insurers are more confident of their ability to manage insurance risks, so their estimate of that risk estimated in the stress tests is for less severe losses than the AM Best view reflected in the BCAR formula. And the opposite is true for investment, particularly equity risk. AM Best's BCAR formula for equity risk is for only a 15% loss, while most insurers who have a stock portfolio had just in 2008 experienced 30% to 40% losses. So insurers are evaluating their investment risk as being much higher than AM Best believes.
Neither set seems to be the complete answer. From looking at these two groups, it makes sense to consider using nine or more categories: premiums, reserves, nat cat, reinsurer credit, bond credit, equities, operational, strategic and liquidity risk. Insurers with multiple large insurance lines may want to add several splits to the premium and reserve categories.
Using Risk Profile for Strategic Planning and Board Discussions
Risk profile can be the focus for bringing enterprise risk into the company’s strategic discussions. The planning process would start with a review of the expected risk profile at the start of the year and look at the impact on risk profile of any major proposed actions as a part of the evaluation of those plans. Each major plan can be discussed regarding whether it increases concentration of risks for the insurer or if it is expected to increase diversification. The risk profile can then be a major communication tool for bringing major management decisions and proposals to the board and to other outside audiences. Each time the risk profile is presented, management can provide explanations of the causes of each significant change in the profile, whether it be from management decisions and actions or because of major changes in the environment.
Risk Profile and Risk Appetite
Once an insurer has a repeatable process in place for portraying enterprise risk as a risk profile, this risk profile can be linked to the risk appetite. The pie charts above focus attention on the relative size of the main types of risks of the insurer. The bar chart below features the sum of the risks. Here the target line represents the expected sum of all of the risks, while the maximum is an aggregate risk limit based upon the risk appetite.
Why are the two risk profiles so different in their views about insurance and investment risks? This author would guess that insurers are more confident of their ability to manage insurance risks, so their estimate of that risk estimated in the stress tests is for less severe losses than the AM Best view reflected in the BCAR formula. And the opposite is true for investment, particularly equity risk. AM Best's BCAR formula for equity risk is for only a 15% loss, while most insurers who have a stock portfolio had just in 2008 experienced 30% to 40% losses. So insurers are evaluating their investment risk as being much higher than AM Best believes.
Neither set seems to be the complete answer. From looking at these two groups, it makes sense to consider using nine or more categories: premiums, reserves, nat cat, reinsurer credit, bond credit, equities, operational, strategic and liquidity risk. Insurers with multiple large insurance lines may want to add several splits to the premium and reserve categories.
Using Risk Profile for Strategic Planning and Board Discussions
Risk profile can be the focus for bringing enterprise risk into the company’s strategic discussions. The planning process would start with a review of the expected risk profile at the start of the year and look at the impact on risk profile of any major proposed actions as a part of the evaluation of those plans. Each major plan can be discussed regarding whether it increases concentration of risks for the insurer or if it is expected to increase diversification. The risk profile can then be a major communication tool for bringing major management decisions and proposals to the board and to other outside audiences. Each time the risk profile is presented, management can provide explanations of the causes of each significant change in the profile, whether it be from management decisions and actions or because of major changes in the environment.
Risk Profile and Risk Appetite
Once an insurer has a repeatable process in place for portraying enterprise risk as a risk profile, this risk profile can be linked to the risk appetite. The pie charts above focus attention on the relative size of the main types of risks of the insurer. The bar chart below features the sum of the risks. Here the target line represents the expected sum of all of the risks, while the maximum is an aggregate risk limit based upon the risk appetite.
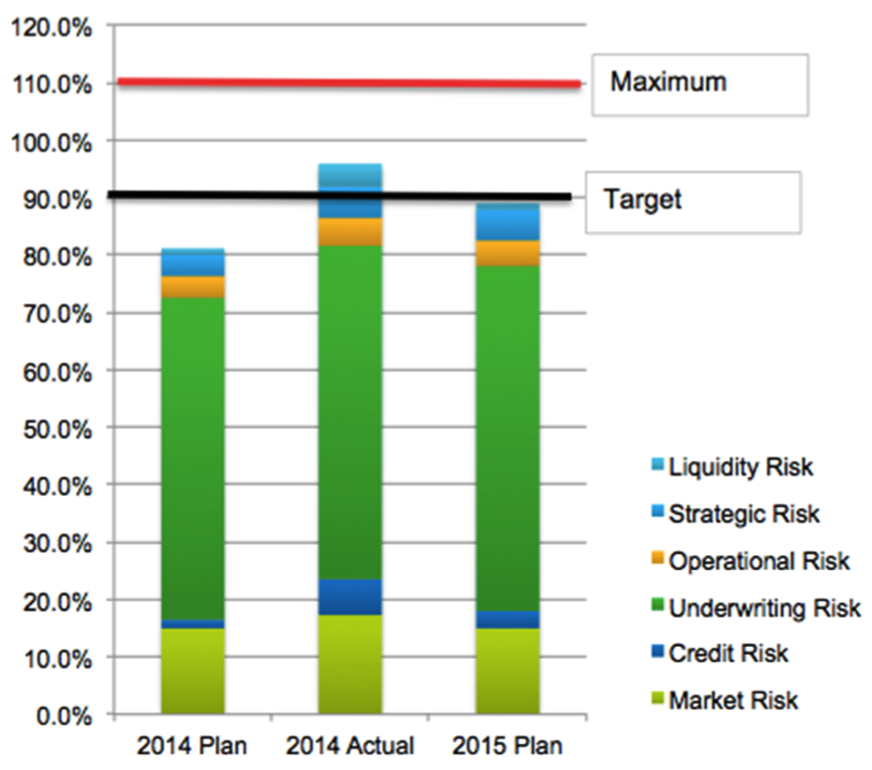 In the example above, the insurer has a target for risk at 90% of a standard (in this case, the standard is for a 400% RBC level; i.e. the target is to have RBC ratio of 440%). The plan is for risk at a level that produces a 480% RBC level, and the maximum tolerance is for risk that would produce a 360% RBC. The 2014 actual risk taking has the insurer at a 420 RBC level, which is above the target but significantly below their maximum. After reviewing the 2014 actual results, management made plans for 2015 that would come in just at the 440% RBC target. That review of the 2014 actual included consideration of the increase in profits associated with the additional risk. When management made the adjustment to reach target for 2015, its first consideration was to reduce less profitable activities. Management was able to make adjustments that significantly improve return for risk taking at a fully utilized level of operation.
In the example above, the insurer has a target for risk at 90% of a standard (in this case, the standard is for a 400% RBC level; i.e. the target is to have RBC ratio of 440%). The plan is for risk at a level that produces a 480% RBC level, and the maximum tolerance is for risk that would produce a 360% RBC. The 2014 actual risk taking has the insurer at a 420 RBC level, which is above the target but significantly below their maximum. After reviewing the 2014 actual results, management made plans for 2015 that would come in just at the 440% RBC target. That review of the 2014 actual included consideration of the increase in profits associated with the additional risk. When management made the adjustment to reach target for 2015, its first consideration was to reduce less profitable activities. Management was able to make adjustments that significantly improve return for risk taking at a fully utilized level of operation.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Dave Ingram is a member of Willis Re's analytics team based in New York. He assists clients with developing their first ORSA (own risk and solvency assessment), presenting their ERM programs to rating agencies, developing and enhancing ERM programs and developing and using economic capital models.
Wearables could improve health monitoring and safety, but issues like battery life, transparency and simplicity need to be resolved.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

As a renown workers’ compensation expert and industry thought leader for 40 years, Jeff Pettegrew seeks to promote and improve understanding of the advantages of the unique Texas alternative injury benefit plan through active engagement with industry and news media as well as social media.
This article, the third in a series, says there is a hard way (crises) or an easy way (risk appetite frameworks) to find the right level.

 Maintaining a risk appetite framework will thus, before the end of this decade, be a matter of necessity, and not a matter of choice. The driver in this regard will be the pace of change. Look at the pictures above, both at a papal blessing, and you see what a difference less than a decade years can make.
What is leading organizations to put formal risk appetite frameworks in place?
Greater investor and regulatory focus, combined with a recognition that risk practices are becoming increasingly professional, has caused organizations to change attitude toward risk from a broadly negative stance to a more positive and engaged approach.
We note a global scarcity of skilled chief risk officers and unwillingness by organizations to commit resources in the current economic climate. Nevertheless, enlightened organizations are gaining appreciation of the links between risk and strategy and in turn toward putting in place the necessary resources and supports to provide greater risk professionalism.
How are risk appetite and strategy related?
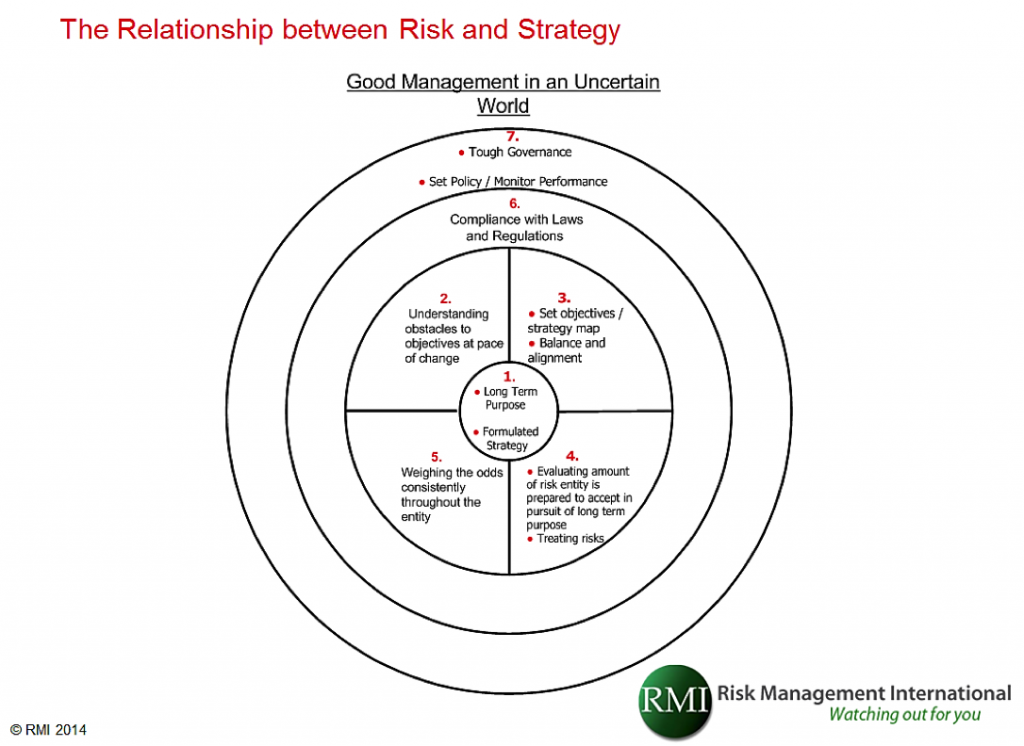
The diagram below describes the relationship.
Maintaining a risk appetite framework will thus, before the end of this decade, be a matter of necessity, and not a matter of choice. The driver in this regard will be the pace of change. Look at the pictures above, both at a papal blessing, and you see what a difference less than a decade years can make.
What is leading organizations to put formal risk appetite frameworks in place?
Greater investor and regulatory focus, combined with a recognition that risk practices are becoming increasingly professional, has caused organizations to change attitude toward risk from a broadly negative stance to a more positive and engaged approach.
We note a global scarcity of skilled chief risk officers and unwillingness by organizations to commit resources in the current economic climate. Nevertheless, enlightened organizations are gaining appreciation of the links between risk and strategy and in turn toward putting in place the necessary resources and supports to provide greater risk professionalism.
How are risk appetite and strategy related?
The diagram below describes the relationship.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Peadar Duffy is founder and chairman of Risk Management International (RMI) a firm that has been advising clients in relation to risk in Ireland and internationally for more than 20 years. He is a member of the International Organisation for Standardization (ISO) TC 262 Working Group 2, which is currently undertaking a review of the global standard for risk management (ISO 31000).
Google's moves toward offering driverless taxis shows just how fraught a transition to a new business model can be.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Chunka Mui is the co-author of the best-selling Unleashing the Killer App: Digital Strategies for Market Dominance, which in 2005 the Wall Street Journal named one of the five best books on business and the Internet. He also cowrote Billion Dollar Lessons: What You Can Learn from the Most Inexcusable Business Failures of the Last 25 Years and A Brief History of a Perfect Future: Inventing the World We Can Proudly Leave Our Kids by 2050.
Workplaces must appreciate that unhappy employees don’t wake up one morning consumed with retaliation. They don’t!

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Felix Nater is the president of Nater Associates and a consummate professional who brings passion to his work as a certified security consultant. He takes time to listen. He is a problem solver, an effective communicator and more than a security consultant.
Sometimes a lack of growth really isn't your fault, but here are ways to slap down a half-dozen common excuses.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Alan Shulman is the publisher of Agency Ideas newsletter, a creative subscription-only sales and marketing trade publication for growing property and casualty agencies. He was a successful P&C producer and agency partner in Western New York for 17 years before launching his popular newsletter in 1990.
Savings were $136 per member per month -- but the wellness/lifestyle management part of the program lost lots of money.

The second-most read article from Health Affairs in 2014 was a fantastic piece by the employee benefits professionals from Pepsi and researchers from the RAND Corp.
The Pepsi team and the RAND researchers evaluated PepsiCo’s wellness program over a seven-year period and found the following:
The article concludes that "blanket statements like ‘wellness saves money’ are not warranted."
As employers evaluate their healthcare strategies, it is important to keep these findings in mind.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|
You must factor in competing national cultures, sub-cultures, Maslow’s theory on self-actualization and the informal groups in the company.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Horst Simon has been in commercial banking and the risk management consultancy industries for four decades. Since 2010 he is a risk management consultant and trainer and was associated with leading global players in the field of risk management consultancy and training as well as business process outsourcing.
The CIO has reached a tipping point: Nearly half of IT spending is now outside her budget. How should CIOs respond?

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Chris Curran is a principal and chief technologist for PwC's advisory practice in the U.S. Curran advises senior executives on their most complex and strategic technology issues and has global experience in designing and implementing high-value technology initiatives across industries.