Geopolitical Goals for Healthcare Hacking?
Are China and other nations conducting hacking campaigns to steal intellectual property and jump start domestic healthcare systems?

Are China and other nations conducting hacking campaigns to steal intellectual property and jump start domestic healthcare systems?

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Byron Acohido is a business journalist who has been writing about cybersecurity and privacy since 2004, and currently blogs at LastWatchdog.com.
Predictive analytics encourage employers to fast-track many workers' comp claims, but they should presume problems are lurking.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Barry Thompson is a 35-year-plus industry veteran. He founded Risk Acuity in 2002 as an independent consultancy focused on workers’ compensation. His expert perspective transcends status quo to build highly effective employer-centered programs.
Drug prices, under physician dispensing, have come down significantly after reforms but remain much higher than at retail pharmacies.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Mark Walls is the vice president, client engagement, at Safety National.
He is also the founder of the Work Comp Analysis Group on LinkedIn, which is the largest discussion community dedicated to workers' compensation issues.
As workers' comp claims dwindle, providers should offer "absence management" -- handling loss of work time for any reason, not just injury.

American employers will dispatch hundreds of staff members to an April gathering in Washington, DC, on corporate compliance issues. In all likelihood, hardly any CEOs in the workers’ comp industry are fluent in these issues, even though by the end of this decade they may change the direction of the workers’ comp businesses, separating the successful from the laggards. A change for workers’ comp leaders hides in plain sight.
Claims have been declining in frequency by about 3.5% a year. It’s prudent to expect continued decline, as jobs become safer every year. Average claims costs, which used to bump up by more than 5% a year, aren’t growing beyond a few percent. Meanwhile, the typical employer’s agendas of employee leave, disability management and wellness have been surging in scope and complexity.
A few workers’ comp companies have already repositioned themselves to provide a broad array of solutions for these agendas. Most workers’ comp CEOs appear to think these burgeoning workplace concerns have little to do with their company’s future. They may be right. Or they may be whistling past the graveyard.
Since the beginning of the Great Recession, demographic, technology and legal trends visible in recent decades began to accelerate in the direction of smaller work injury risk and larger non-occupational employee risks. Frank Neuhauser of the University of California at Berkeley estimated that for most workers it is more dangerous to drive to work than to be at work.
And notice the rise in employee leave benefits and the greater emphasis on wellness (despite deserved criticism of overselling that concept). Perhaps this is how Occupy Wall Street ends: not in a revolutionary bang, but a paid parental leave benefit and a worksite yoga studio.
The Disability Management Employer Coalition puts on the April conference as its annual problem-solving exercise for the Family and Medical Leave Act and Americans with Disabilities Act. In addition to these federal mandates, states and localities have been promulgating leave-related mandates by the dozens. In January, for instance, Tacoma, WA, enacted a law requiring employers to offer at least three days of paid sick leave come January 2015. ClaimVantage, which sells absence management software, reports there are about 140 federal and state family leaves across the nation. When adding ancillary leaves like jury duty and blood donor leaves, the numbers rise to about 400.
Paid family leave is gaining momentum to become a mandated benefit. The U.S. is the only high-earning country that does not offer paid leave after the birth of a child and only one of eight countries in the world that doesn't mandate paid leave for new mothers.
According to the Integrated Benefits Institute, workers’ comp accounts for a mere 11% of all work absences involving a medical condition. Legally mandated and voluntary benefits, disability accommodation, wellness and other employee-centric programs have by intertwining themselves raised their visibility in corporate C-Suites. No single, memorable descriptor today captures them successfully.
Phrases such as “health and productivity management” and “total health” are bandied about. I suggest a simple term, “absence management,” in a report I wrote called “Seismic Shifts: An Essential Guide for Practitioners and CEOs in Workers' Comp,” which WorkCompCentral published in February.
The absence business beckons
Although the labels will evolve, the need of employers for expert outside assistance to address their agendas is bound to grow. Will workers’ comp companies deliver solutions?
The employers most ready to ask for help include those with relatively large workers’ comp costs to begin with: middle- to large-sized employers. Workers' comp claims payers today will process about $65 billion in workers' comp benefits this year. Perhaps 15% of these benefits involve very large employers. A further 25% involve employers that are not that large yet incur workers’ comp losses of about $200,000 a year or more.
Combined, these employers account for 45% of workers’ comp benefits. In other words, about half of the workers’ comp business today is with employers big enough to know they have a complicated absence management problem on their hands. Their human resource executives and legal counsel have been telling CEOs that the compliance risks of government mandates can’t be ignored. The mandates have grown into an elephantine mass so thick that without expert outside assistance an employer has a high probability – say, 100% -- of violating some law or other.
The more alert and early-adapting segment of employers tends to affiliate with the San Francisco-based Integrate Benefits Institute. Their individual staff members join the San Diego-based Disability Management Employer Coalition. These membership organizations feed the demand for training, resource networking and applied research. Broadspire, ESIS, Sedgwick, York and perhaps other third-party administrators already market services to manage at least some aspect of non-occupational absences. Workers' comp claims payers can manage non-occupational absences because they already possess the needed core competencies.
Pared down to the essentials, the workers' comp claims payer does six things:
Absence management does basically the same things. Further tying together workers’ comp and non-occupational absences in a workforce is the vital role of health behaviors of employees. The workers’ comp claims executive is acutely aware that health behaviors of injured workers often drive up claims costs. It is increasingly clear that smoking can be a more costly unsafe act than, say, distraction. Not that smoking precipitates an occupational or non-occupational injury (there’s scanty evidence of that), but that smokers are at more sharply higher risk to heal slowly and to become dependent on opioids in treatment.
The Integrated Benefits Institute has for years carefully analyzed patterns in non-occupational absences. It says that employers can and should use a coherent master plan for absences of all kinds, wellness initiatives and claims management.
In a phone and email exchange, IBI President Tom Parry suggests that workers’ comp claims payers think through their strengths in medical care, disability management and return to work.
“These all are key parts to an employer’s strategy in taking a comprehensive approach to lost work time management,” he says. Also, he advises, be prepared to benchmark and compare. Get hold of industry-specific benchmarking data across lost time programs, workers’ comp, FMLA and short and long-term disability. Become fluent in plan design terminology on the non-occupational side. Review the research literature on the cross-program impacts of health and a total absence management approach. IBI just published research on claims migration across programs, “Crossing Over -- Do Benefits and Risk Managers Have Anything to Talk About?”
Why companies may hold back
A workers’ comp claims payer might not enter the absence business because it does not believe that the workers’ comp industry is shrinking. For instance, the average cost of claims may, as it has in the past, grow faster than the reduction in injuries, leaving claims payers with an ever-larger pie.
But in recent years average indemnity and medical costs have greatly slowed their growth and in some jurisdictions declined. And the incidence of lost time compensable claims continues to decline, the one clear exception being the island of all exceptions, Southern California.
Also, workers’ comp executives might say there is no apparent demand from their clients for non-occupational services. This sort of flies in the face of the experience of TPAs that have launched non-occupational service units. (True, they focus on the higher end of the employer market.) But the observation also doesn’t jibe with the workers’ comp industry’s experience with emerging services in the past.
In instances of innovation, from medical bill review to pharmacy management to Medicare set-asides, large-scale and profitable services emerged after initial years of puzzlement. The fog banks eventually lift.
Then there are impediments in the broker community. It’s almost inevitable that absence management involves insurance products sold through benefits brokers and products sold through property and casualty brokers. They don’t talk a lot, even when working under the same roof. This complicates the work of product design and marketing.
Another reason to say no to opportunity is the challenging learning curve that absence management brings. But look at how the TPAs handled that. Those that have expanded their service offerings beyond workers’ comp claims all appear to forge alliances with, or acquire, servicing partners already steeped in some aspect of absence management.
It may be too harsh to equate workers' comp claims payers with the railroad industry, which 60 years ago asserted that it was in the railroad, not the transportation, business. Perhaps too harsh, but there may be a lesson in that story.
The decline of work injuries
Injuries requiring at least 31 days away from work
| year | 1993 | 2015 | 2022 (projected) |
| injuries | 450,000 | 250,000 | 175,000 |
| Total employment | 110 million | 133 million | 148 million |
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Many companies focus on the wrong thing. More data isn't better. The right data is better -- and can greatly improve the customer experience.

What’s the big deal about big data? Big data is an enormously appealing subject these days. However, many companies miss the big picture when collecting it -- or drowning in it. There is an idea that the more data, the better. In fact, the focus should be on determining the right data to help improve the overall customer experience. Raining Big Data Big data is like the weather -- we’re talking about it, but we haven’t quite figured out how to do anything about it. Even fewer know how to leverage it. There are lots of questions but few answers. For example, who’s familiar with the 3Vs? But don’t be afraid to get wet. Data can be used to improve many things for many people – including your employees and customers. I say “can” because, before you do anything, you need to make sure you are using the right data -- and not just the random troves collected throughout the years. Mining the right data can lead you to the right customer problems, which can then be solved, creating a better customer experience. Background Checks Always define before measuring. What does great customer experience look like in your industry? Figure out what you need to do to wow customers and then compare that with the reality of your business as it stands now. I’ve utilized customer journey mapping, net promoter scores and voice of the customer metrics with great results. You can even provide customers incentives to help you out with input. Here’s a smart way to do that. Start by checking the leading survey on customer experience, the Forrester Customer Experience Index, to see where your organization lands. It might surprise you. Reliable Friends Are Powerful Friends Right data helps organizations do many things, including: • Anticipate what customers want before they ask for it • Identify customer pain points and resolve them • Create new business value • Improve customer service interactions • Develop more effective marketing and better products • Improve operational efficiencies Take Southwest Airlines. It's using speech analytics to extract data-rich info from live-recorded interactions between customers and personnel to get a better understanding of customers. Or read about Avis Budget’s data-driven growth model. It uses big data to identify the most valuable customers today and tomorrow. How, you ask? By examining a broad range of data sources, including structured information like purchase histories, CRM data and intelligence from industry partners, as well as unstructured information like social media, blogs and videos. Sorting through the data has helped all customers be treated like VIPs. These are only two examples of forward-thinking leaders using the right data to create actionable insights that monetize their data. There are many more. What about your competitors? How far along are they down the big data road? And are they using the right data?
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Donna Peeples is chief customer officer at Pypestream, which enables companies to deliver exceptional customer service using real-time mobile chatbot technology. She was previously chief customer experience officer at AIG.
With so much contention appearing in what was supposed to be a no-fault system, is it time to redesign work comp from scratch?

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

As a renown workers’ compensation expert and industry thought leader for 40 years, Jeff Pettegrew seeks to promote and improve understanding of the advantages of the unique Texas alternative injury benefit plan through active engagement with industry and news media as well as social media.
The market has become tough for those buying management liability insurance -- and may get even tougher.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Laura Zaroski is the vice president of management and employment practices liability at Socius Insurance Services. As an attorney with expertise in employment practices liability insurance, in addition to her role as a producer, Zaroski acts as a resource with respect to Socius' employment practices liability book of business.
Risk leaders must make themselves essential to others' successes, earning the kinds of points that count among the business' leaders.

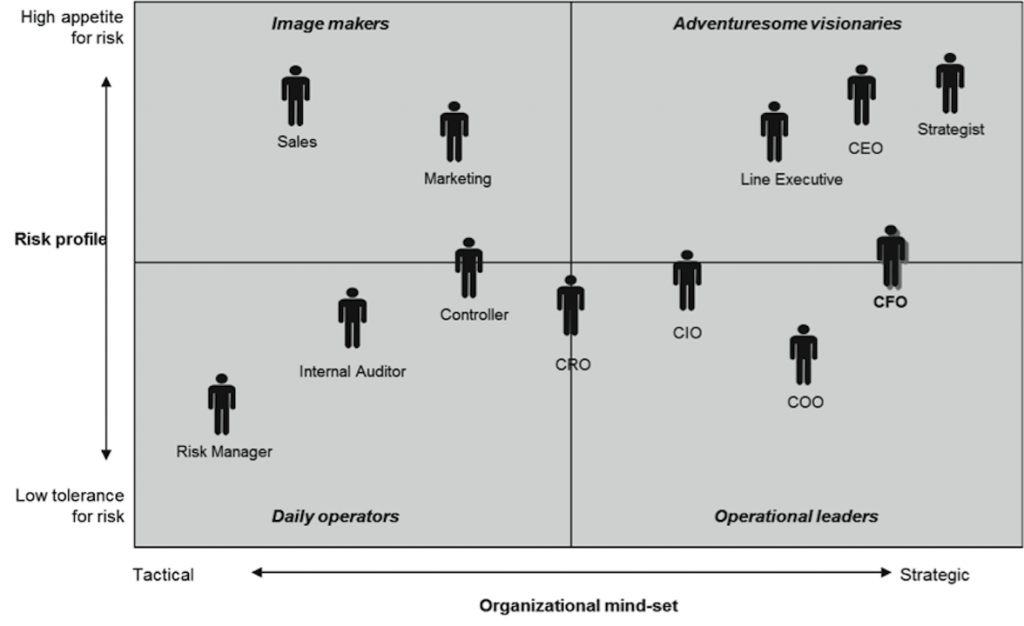 The chart above, from The Global CFO Study 2008: Balancing Risk and Performance Within an Integrated Finance Organization, reflects that risk managers, even chief risk officers, are perceived by chief financial officers as more tactical in mindset than strategic.
Never fear: Perceptions can be changed .
The chart above, from The Global CFO Study 2008: Balancing Risk and Performance Within an Integrated Finance Organization, reflects that risk managers, even chief risk officers, are perceived by chief financial officers as more tactical in mindset than strategic.
Never fear: Perceptions can be changed .
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Christopher E. Mandel is senior vice president of strategic solutions for Sedgwick and director of the Sedgwick Institute. He pioneered the development of integrated risk management at USAA.
Insurance brands are generally trusted, but it's time for a refresh.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Nigel Walsh is a partner at Deloitte and host of the InsurTech Insider podcast. He is on a mission to make insurance lovable.
He spends his days:
Supporting startups. Creating communities. Building MGAs. Scouting new startups. Writing papers. Creating partnerships. Understanding the future of insurance. Deploying robots. Co-hosting podcasts. Creating propositions. Connecting people. Supporting projects in London, New York and Dublin. Building a global team.
SWOT (strengths, weaknesses, opportunities and threats) often fails to look hard enough at how risks can cascade through connected systems.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

David Patrishkoff is president of E3 (Extreme Enterprise Efficiency) and the founder of the Institute for Cascade Effect Research. He is a Lean Six Sigma Master Black Belt and the inventor of a cascading risk management methodology that has patent pending status.