Moving to Real-Time Risk Management
Historically, policies are periodic, but risk is continuous. Now, as an auto insurer shows, technology allows for real-time risk management.

Historically, policies are periodic, but risk is continuous. Now, as an auto insurer shows, technology allows for real-time risk management.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Mike Fitzgerald is a senior analyst with Celent's insurance practice. He has specific expertise in property/casualty automation, operations management and insurance product development. his research focuses on innovation, insurance business processes and operations, social media and distribution management.
The debt problems in Greece show a flaw in the euro and underscore the need for investors to pay attention to relative currency movements.

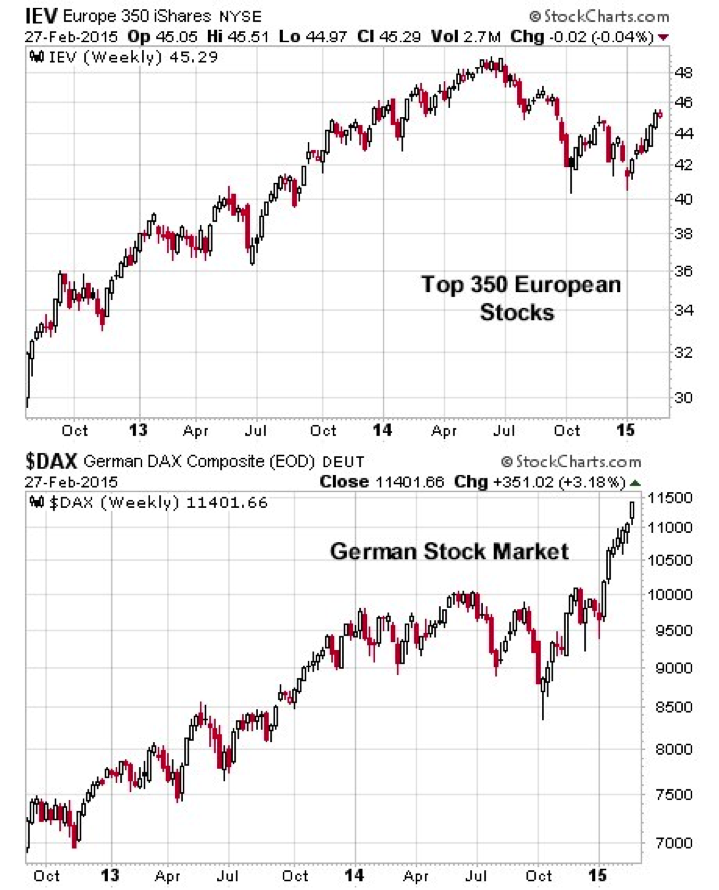 Broadly, euro area equities have not yet attained the highs seen in 2014. But German stocks are close to 15% ahead of their 2014 highs. Why? Germany is seen as the most fiscally prudent and financially strong of the euro members. What we are seeing is capital gravitating toward the perception of safety that is Germany, relative to the euro area as a whole. This is the type of capital flow analysis that is so important in the current environment.
The headline media portray the Greek problem as just another country living beyond its means and unable to repay the debts it has accumulated. But the real issues involved are so much more meaningful. They cut to the core of euro viability as a currency and stability in the broad euro banking system. The Greek problem's resurfacing in the last six months has necessarily pressured the euro as a currency and triggered an internal move of equity capital from the broad euro equity markets to individual countries perceived as strong, such as Germany. This is exactly the theme we have been discussing for months. Global capital is seeking refuge from currency debasement and principal safety in the financial markets of countries with strong balance sheets. For now, the weight and movement of global capital remains an important element of our analytical framework.
Watching outcomes ahead for Greece within the context of the greater Eurozone will be important. Greece truly is a Petri dish for what may be to come for greater Europe. Outcomes will affect the euro as a currency, the reality of the Greek economy, the perceived integrity of the European banking system and both domestic and global euro-driven capital flows. For now, Greece is the word.
Broadly, euro area equities have not yet attained the highs seen in 2014. But German stocks are close to 15% ahead of their 2014 highs. Why? Germany is seen as the most fiscally prudent and financially strong of the euro members. What we are seeing is capital gravitating toward the perception of safety that is Germany, relative to the euro area as a whole. This is the type of capital flow analysis that is so important in the current environment.
The headline media portray the Greek problem as just another country living beyond its means and unable to repay the debts it has accumulated. But the real issues involved are so much more meaningful. They cut to the core of euro viability as a currency and stability in the broad euro banking system. The Greek problem's resurfacing in the last six months has necessarily pressured the euro as a currency and triggered an internal move of equity capital from the broad euro equity markets to individual countries perceived as strong, such as Germany. This is exactly the theme we have been discussing for months. Global capital is seeking refuge from currency debasement and principal safety in the financial markets of countries with strong balance sheets. For now, the weight and movement of global capital remains an important element of our analytical framework.
Watching outcomes ahead for Greece within the context of the greater Eurozone will be important. Greece truly is a Petri dish for what may be to come for greater Europe. Outcomes will affect the euro as a currency, the reality of the Greek economy, the perceived integrity of the European banking system and both domestic and global euro-driven capital flows. For now, Greece is the word.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Brian Pretti is a partner and chief investment officer at Capital Planning Advisors. He has been an investment management professional for more than three decades. He served as senior vice president and chief investment officer for Mechanics Bank Wealth Management, where he was instrumental in growing assets under management from $150 million to more than $1.4 billion.
Ideally, anti-rebating laws shouldn't exist, but a personal story shows how consumers need a certain level of protection from dirtbags.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Joel Wood is senior vice president of government affairs at the Council of Insurance Agents & Brokers, a position he has held since 1992. Dubbed one of the top trade association lobbyists in Washington by “The Hill,” Wood is a regular contributor to Leader's Edge magazine.
Google Compare just adds to the illusion that consumers really can compare insurance products and reach purchasing decisions online.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

William C. Wilson, Jr., CPCU, ARM, AIM, AAM is the founder of Insurance Commentary.com. He retired in December 2016 from the Independent Insurance Agents & Brokers of America, where he served as associate vice president of education and research.
Google dominates in customer experience, Amazon in supply chain, Apple in the experience and Facebook in community -- disruption is coming!

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Nigel Walsh is a partner at Deloitte and host of the InsurTech Insider podcast. He is on a mission to make insurance lovable.
He spends his days:
Supporting startups. Creating communities. Building MGAs. Scouting new startups. Writing papers. Creating partnerships. Understanding the future of insurance. Deploying robots. Co-hosting podcasts. Creating propositions. Connecting people. Supporting projects in London, New York and Dublin. Building a global team.
Insurers must start with a single view of the customer -- which only about a quarter now have -- but then build a fully 720-degree view of each individual.

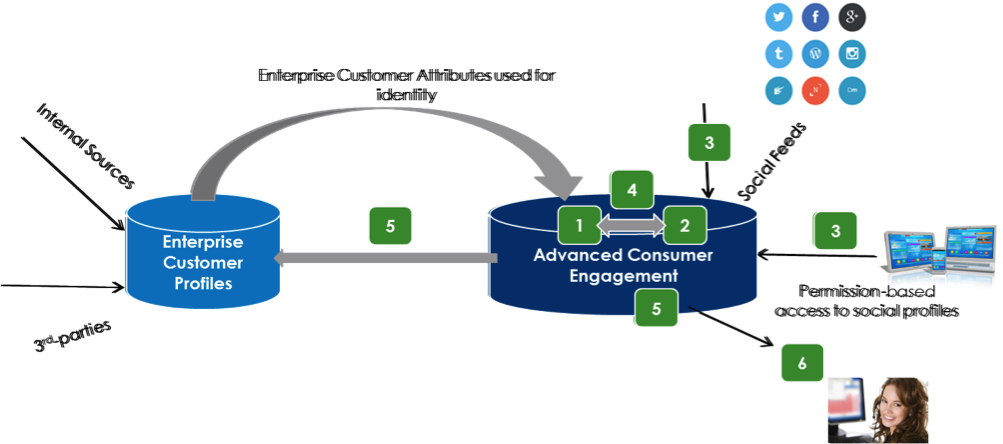 The 360-degree view is essential for improving both bottom-line and top-line performance. Reliable, unified customer views enable major gains in customer service (retention) and marketing effectiveness (cross-sell and upsell), not to mention claims and fraud. The consumer 360 was the backbone and first step one insurer took to drive cross-sales revenue. This large insurance and financial services firm was able to quantify marketing effectiveness and audience behavior, enabling the company to make informed tactical decisions that ensure more efficient marketing spending.
In this case, the development and implementation of closed-loop marketing analytics across key enterprise business units, utilizing predictive models, segmentation algorithms, churn analysis, modeling and funnel analysis, delivered the ability to continuously analyze and understand data from more than 25 million customers and prospects every week. With 360-degree customer views, insights can be delivered from data that allow this insurer to clearly see how enterprise marketing efforts can improve cross-sell and boost revenues.
Personalization
Once an insurer has a reliable customer view, the work of improving customer experience and satisfaction can begin. Consumers value personalized experience. Two-thirds of consumers are more likely to trust and engage with brands that allow them to customize and share personalization and contact preferences. More than half of consumers feel more positive about a brand when messages are personalized. According to Harris Interactive, 86% of consumers quit doing business with a company because of a bad customer experience, up from 59% four years ago. That statistic should serve as a wake-up call to invest in personalization -- the key to enhancing consumer engagement.
Implementing advanced consumer engagement (ACE) via a variety of data management and analytic strategies and solutions, there are five key elements of personalization:
The 360-degree view is essential for improving both bottom-line and top-line performance. Reliable, unified customer views enable major gains in customer service (retention) and marketing effectiveness (cross-sell and upsell), not to mention claims and fraud. The consumer 360 was the backbone and first step one insurer took to drive cross-sales revenue. This large insurance and financial services firm was able to quantify marketing effectiveness and audience behavior, enabling the company to make informed tactical decisions that ensure more efficient marketing spending.
In this case, the development and implementation of closed-loop marketing analytics across key enterprise business units, utilizing predictive models, segmentation algorithms, churn analysis, modeling and funnel analysis, delivered the ability to continuously analyze and understand data from more than 25 million customers and prospects every week. With 360-degree customer views, insights can be delivered from data that allow this insurer to clearly see how enterprise marketing efforts can improve cross-sell and boost revenues.
Personalization
Once an insurer has a reliable customer view, the work of improving customer experience and satisfaction can begin. Consumers value personalized experience. Two-thirds of consumers are more likely to trust and engage with brands that allow them to customize and share personalization and contact preferences. More than half of consumers feel more positive about a brand when messages are personalized. According to Harris Interactive, 86% of consumers quit doing business with a company because of a bad customer experience, up from 59% four years ago. That statistic should serve as a wake-up call to invest in personalization -- the key to enhancing consumer engagement.
Implementing advanced consumer engagement (ACE) via a variety of data management and analytic strategies and solutions, there are five key elements of personalization:
 Choose platforms that will allow you to grow by scaling hardware, rather than doing costly rewrites. Assume that your next step is market domination. This allows the enterprise to focus on innovative customer experiences rather than performance tuning.
Choose platforms that will allow you to grow by scaling hardware, rather than doing costly rewrites. Assume that your next step is market domination. This allows the enterprise to focus on innovative customer experiences rather than performance tuning.
 Invest in architecture and standards that enable agility. Solutions should be as simple as possible.
Invest in architecture and standards that enable agility. Solutions should be as simple as possible.
 Quality should always trump quantity, when it comes to data. Value your data by focusing on core data-quality issues, first. Information will always be more valuable to your consumers than data. Reliable information comes from quality data in context.
Quality should always trump quantity, when it comes to data. Value your data by focusing on core data-quality issues, first. Information will always be more valuable to your consumers than data. Reliable information comes from quality data in context.
 Position your ACE program to engage with consumers and quickly adapt to consumer feedback. Build in processes to show you value consumer feedback. Provide updates and enhancements quickly in smaller releases, continually enhancing the customer experience. By 2020, the customer will manage 85% of the relationship with an enterprise without interacting with a human, according to Gartner. There is plenty of room for improvement via quick iteration, especially in the realm of customer self-service.
Position your ACE program to engage with consumers and quickly adapt to consumer feedback. Build in processes to show you value consumer feedback. Provide updates and enhancements quickly in smaller releases, continually enhancing the customer experience. By 2020, the customer will manage 85% of the relationship with an enterprise without interacting with a human, according to Gartner. There is plenty of room for improvement via quick iteration, especially in the realm of customer self-service.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Kay Morscheiser is a strategic leader with more than 25 years of experience leveraging strategy, operations and data, creating market-leading, profitable organizations. Currently the insurance practice leader at Clarity Solution Group, she is responsible for setting direction and solution creation from ideation through implementation and execution.
Are China and other nations conducting hacking campaigns to steal intellectual property and jump start domestic healthcare systems?

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Byron Acohido is a business journalist who has been writing about cybersecurity and privacy since 2004, and currently blogs at LastWatchdog.com.
Predictive analytics encourage employers to fast-track many workers' comp claims, but they should presume problems are lurking.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Barry Thompson is a 35-year-plus industry veteran. He founded Risk Acuity in 2002 as an independent consultancy focused on workers’ compensation. His expert perspective transcends status quo to build highly effective employer-centered programs.
Drug prices, under physician dispensing, have come down significantly after reforms but remain much higher than at retail pharmacies.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Mark Walls is the vice president, client engagement, at Safety National.
He is also the founder of the Work Comp Analysis Group on LinkedIn, which is the largest discussion community dedicated to workers' compensation issues.
As workers' comp claims dwindle, providers should offer "absence management" -- handling loss of work time for any reason, not just injury.

American employers will dispatch hundreds of staff members to an April gathering in Washington, DC, on corporate compliance issues. In all likelihood, hardly any CEOs in the workers’ comp industry are fluent in these issues, even though by the end of this decade they may change the direction of the workers’ comp businesses, separating the successful from the laggards. A change for workers’ comp leaders hides in plain sight.
Claims have been declining in frequency by about 3.5% a year. It’s prudent to expect continued decline, as jobs become safer every year. Average claims costs, which used to bump up by more than 5% a year, aren’t growing beyond a few percent. Meanwhile, the typical employer’s agendas of employee leave, disability management and wellness have been surging in scope and complexity.
A few workers’ comp companies have already repositioned themselves to provide a broad array of solutions for these agendas. Most workers’ comp CEOs appear to think these burgeoning workplace concerns have little to do with their company’s future. They may be right. Or they may be whistling past the graveyard.
Since the beginning of the Great Recession, demographic, technology and legal trends visible in recent decades began to accelerate in the direction of smaller work injury risk and larger non-occupational employee risks. Frank Neuhauser of the University of California at Berkeley estimated that for most workers it is more dangerous to drive to work than to be at work.
And notice the rise in employee leave benefits and the greater emphasis on wellness (despite deserved criticism of overselling that concept). Perhaps this is how Occupy Wall Street ends: not in a revolutionary bang, but a paid parental leave benefit and a worksite yoga studio.
The Disability Management Employer Coalition puts on the April conference as its annual problem-solving exercise for the Family and Medical Leave Act and Americans with Disabilities Act. In addition to these federal mandates, states and localities have been promulgating leave-related mandates by the dozens. In January, for instance, Tacoma, WA, enacted a law requiring employers to offer at least three days of paid sick leave come January 2015. ClaimVantage, which sells absence management software, reports there are about 140 federal and state family leaves across the nation. When adding ancillary leaves like jury duty and blood donor leaves, the numbers rise to about 400.
Paid family leave is gaining momentum to become a mandated benefit. The U.S. is the only high-earning country that does not offer paid leave after the birth of a child and only one of eight countries in the world that doesn't mandate paid leave for new mothers.
According to the Integrated Benefits Institute, workers’ comp accounts for a mere 11% of all work absences involving a medical condition. Legally mandated and voluntary benefits, disability accommodation, wellness and other employee-centric programs have by intertwining themselves raised their visibility in corporate C-Suites. No single, memorable descriptor today captures them successfully.
Phrases such as “health and productivity management” and “total health” are bandied about. I suggest a simple term, “absence management,” in a report I wrote called “Seismic Shifts: An Essential Guide for Practitioners and CEOs in Workers' Comp,” which WorkCompCentral published in February.
The absence business beckons
Although the labels will evolve, the need of employers for expert outside assistance to address their agendas is bound to grow. Will workers’ comp companies deliver solutions?
The employers most ready to ask for help include those with relatively large workers’ comp costs to begin with: middle- to large-sized employers. Workers' comp claims payers today will process about $65 billion in workers' comp benefits this year. Perhaps 15% of these benefits involve very large employers. A further 25% involve employers that are not that large yet incur workers’ comp losses of about $200,000 a year or more.
Combined, these employers account for 45% of workers’ comp benefits. In other words, about half of the workers’ comp business today is with employers big enough to know they have a complicated absence management problem on their hands. Their human resource executives and legal counsel have been telling CEOs that the compliance risks of government mandates can’t be ignored. The mandates have grown into an elephantine mass so thick that without expert outside assistance an employer has a high probability – say, 100% -- of violating some law or other.
The more alert and early-adapting segment of employers tends to affiliate with the San Francisco-based Integrate Benefits Institute. Their individual staff members join the San Diego-based Disability Management Employer Coalition. These membership organizations feed the demand for training, resource networking and applied research. Broadspire, ESIS, Sedgwick, York and perhaps other third-party administrators already market services to manage at least some aspect of non-occupational absences. Workers' comp claims payers can manage non-occupational absences because they already possess the needed core competencies.
Pared down to the essentials, the workers' comp claims payer does six things:
Absence management does basically the same things. Further tying together workers’ comp and non-occupational absences in a workforce is the vital role of health behaviors of employees. The workers’ comp claims executive is acutely aware that health behaviors of injured workers often drive up claims costs. It is increasingly clear that smoking can be a more costly unsafe act than, say, distraction. Not that smoking precipitates an occupational or non-occupational injury (there’s scanty evidence of that), but that smokers are at more sharply higher risk to heal slowly and to become dependent on opioids in treatment.
The Integrated Benefits Institute has for years carefully analyzed patterns in non-occupational absences. It says that employers can and should use a coherent master plan for absences of all kinds, wellness initiatives and claims management.
In a phone and email exchange, IBI President Tom Parry suggests that workers’ comp claims payers think through their strengths in medical care, disability management and return to work.
“These all are key parts to an employer’s strategy in taking a comprehensive approach to lost work time management,” he says. Also, he advises, be prepared to benchmark and compare. Get hold of industry-specific benchmarking data across lost time programs, workers’ comp, FMLA and short and long-term disability. Become fluent in plan design terminology on the non-occupational side. Review the research literature on the cross-program impacts of health and a total absence management approach. IBI just published research on claims migration across programs, “Crossing Over -- Do Benefits and Risk Managers Have Anything to Talk About?”
Why companies may hold back
A workers’ comp claims payer might not enter the absence business because it does not believe that the workers’ comp industry is shrinking. For instance, the average cost of claims may, as it has in the past, grow faster than the reduction in injuries, leaving claims payers with an ever-larger pie.
But in recent years average indemnity and medical costs have greatly slowed their growth and in some jurisdictions declined. And the incidence of lost time compensable claims continues to decline, the one clear exception being the island of all exceptions, Southern California.
Also, workers’ comp executives might say there is no apparent demand from their clients for non-occupational services. This sort of flies in the face of the experience of TPAs that have launched non-occupational service units. (True, they focus on the higher end of the employer market.) But the observation also doesn’t jibe with the workers’ comp industry’s experience with emerging services in the past.
In instances of innovation, from medical bill review to pharmacy management to Medicare set-asides, large-scale and profitable services emerged after initial years of puzzlement. The fog banks eventually lift.
Then there are impediments in the broker community. It’s almost inevitable that absence management involves insurance products sold through benefits brokers and products sold through property and casualty brokers. They don’t talk a lot, even when working under the same roof. This complicates the work of product design and marketing.
Another reason to say no to opportunity is the challenging learning curve that absence management brings. But look at how the TPAs handled that. Those that have expanded their service offerings beyond workers’ comp claims all appear to forge alliances with, or acquire, servicing partners already steeped in some aspect of absence management.
It may be too harsh to equate workers' comp claims payers with the railroad industry, which 60 years ago asserted that it was in the railroad, not the transportation, business. Perhaps too harsh, but there may be a lesson in that story.
The decline of work injuries
Injuries requiring at least 31 days away from work
| year | 1993 | 2015 | 2022 (projected) |
| injuries | 450,000 | 250,000 | 175,000 |
| Total employment | 110 million | 133 million | 148 million |
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|
