KEY TAKEAWAY:
--Call centers for 911 emergency services are woefully underfunded and understaffed. So are emergency medical technicians (EMTs), which are not considered essential services in 39 states and thus have to be paid for through community fundraisers. The lack of funding needs to be fixed.
----------
The National Emergency Number Association (NENA) recently released a study reporting that over 80% of 911 call centers across the country are understaffed and underfunded. There are simply not enough operators and dispatchers in the 911 system.
For example, Montgomery County in Maryland, which fields 2,200 calls to 911 every day, has seen staffing levels decline 47% in the past year.
The reason revolves around long shifts, mandatory overtime, low pay and abusive behavior faced by the dispatchers.
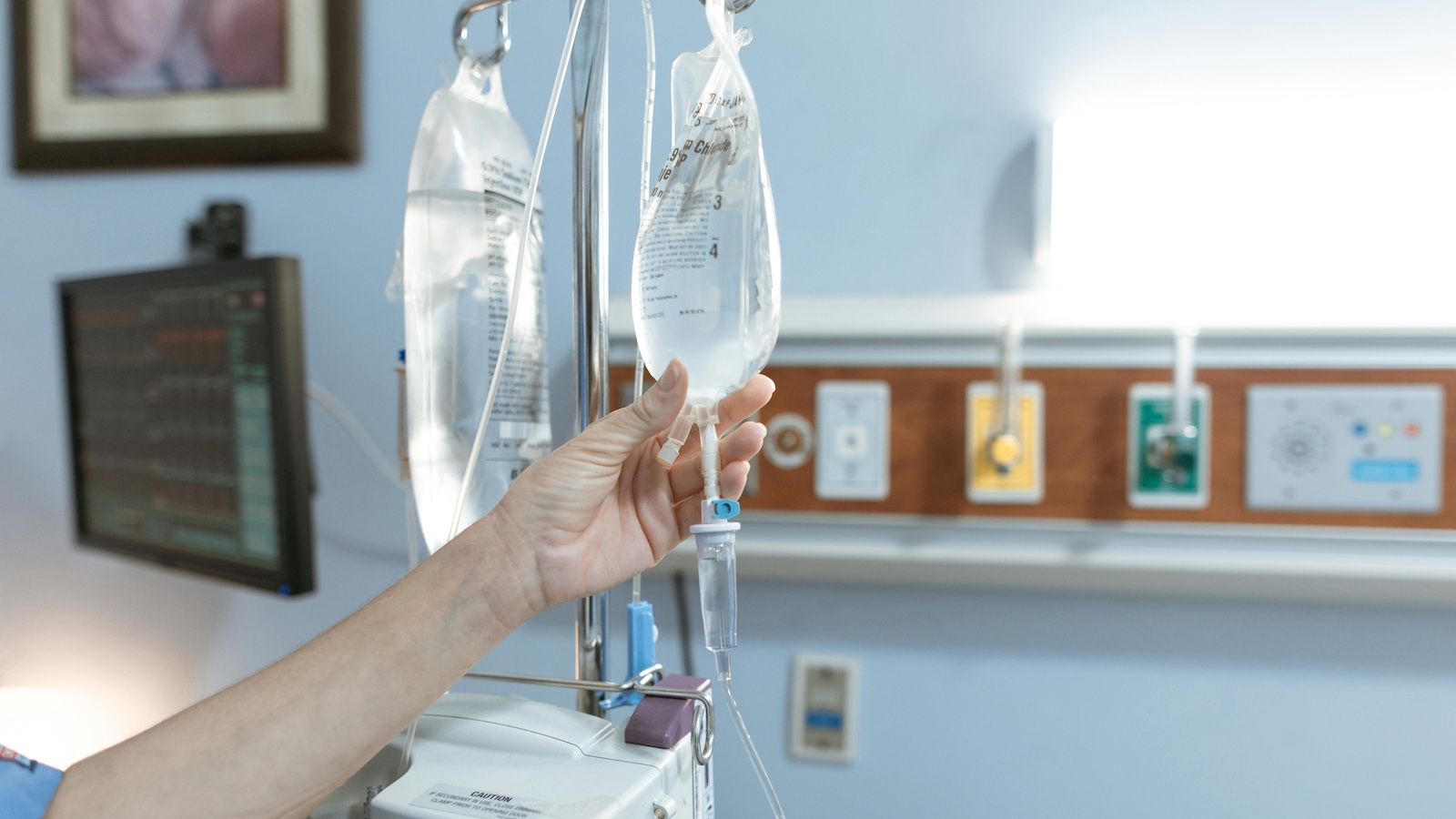
At the same time, there is a shortage of emergency medical technicians (EMTs), especially in rural America. (See, "Fixing the EMT Crisis in Rural America.") The combination puts millions of Americans at risk during a medical emergency, especially in a potential life or death situation. The dual crises severely complicate the long-standing overcrowding and inefficient use of emergency medical services that has been wreaking havoc in emergency departments since long before the COVID-19 pandemic further overwhelmed the system.
According to the Centers for Disease Control and Prevention’s (CDC) most recent statistics, there are 131 million emergency room visits annually in the U.S., with 18.6 million, or roughly 14% of those visits, resulting in hospital admissions. Over 28 million people are taken by ambulance service each year to the local ER, with two-thirds transported by the local fire department or municipal government. Roughly 3 million people per year who are taken by ambulance are in a critical, or even life-and-death situation. Tragically, the majority are due to auto accidents from aggressive and impaired drivers.
See also: What Is 988? Future of Crisis Services
Our healthcare system is the best in the world, but it is simultaneously expensive, wasteful and inefficient, failing to address underlying basic barriers for access to primary healthcare. When the next trillion-dollar budget negotiations begin in Washington, instead of wasting millions on pet projects, federal funding should help state and local governments provide the necessary funding for 911 emergency call center operations around the country with highly paid career opportunities.
And how about funding and training for EMT squads around the country? How about funding for new medical research and technologies, including AI, to diagnose and treat people in emergency medical situations?
I spent my career in employee benefits consulting and have found that virtually everybody understands the need for health insurance, if not for themselves, at least for their families. However, nobody thinks they are going to get in an accident, have a medical emergency or get hurt on the job, even though the CDC reports that one in five Americans will have an emergency room visit each year.
The big picture includes helping address overcrowded ERs and the waste of critical time, money and resources. There are now non-emergency call center operations in some local areas (you dial 311) to free up 911 emergency call center time; these need to be promoted. We need to fund community health centers so people can have access to primary healthcare without going to the local emergency room. Even people with health insurance are having lengthy delays in getting primary healthcare. Recent data show the wait times for new patients is 26 days on average. OBGYN and orthopedic wait times for new patient visits are even longer.
I am delighted to see the growth of local urgent care facilities, which played a huge role in COVID-19 vaccinations, and the growing use of telemedicine – especially given the long waits for primary care visits. But for heaven’s sake, we need to properly fund the 911 call center operations and first responders and EMT squads around the country.
Now.