Predictions for Work Comp in 2015
Medical marijuana will be a non-event; regulators will be more active on medical management, including on the use of drugs; and more....

Medical marijuana will be a non-event; regulators will be more active on medical management, including on the use of drugs; and more....

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Joseph Paduda, the principal of Health Strategy Associates, is a nationally recognized expert in medical management in group health and workers' compensation, with deep experience in pharmacy services. Paduda also leads CompPharma, a consortium of pharmacy benefit managers active in workers' compensation.
Tokio Marine shows how to make the transition from periodic sales and service to a continuous relationship with customers.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Mike Fitzgerald is a senior analyst with Celent's insurance practice. He has specific expertise in property/casualty automation, operations management and insurance product development. his research focuses on innovation, insurance business processes and operations, social media and distribution management.
A seldom-used feature known as the extended reporting period, or ERP, shows how it's possible to spot new trends and ride them.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

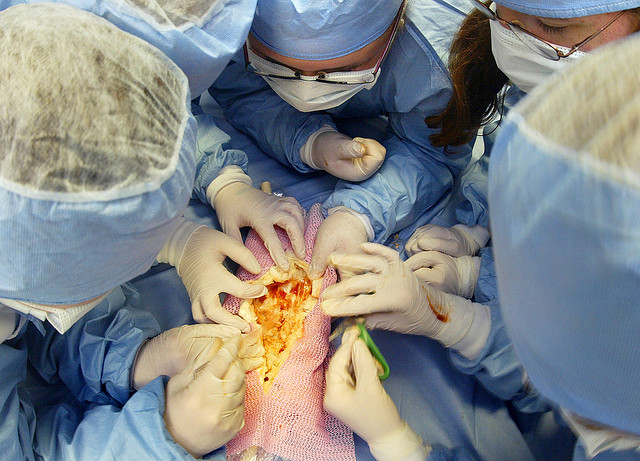
Steve Spina is responsible for OneBeacon Professional Insurance's health group, which provides liability insurance solutions for medical facilities, long-term care facilities, managed care organizations and hospitals, physicians and complex risks. Spina’s group also offers tailored coverages for the medical excess segment and has developed an innovative extended reporting period (ERP) product to address the evolving physicians’ integration environment.
A prominent critic emails a prominent proponent to suggest a letter laying out the common ground -- but receives no reponse.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|
Centralizing the capabilities devoted to customer insight can produce efficiency but also carries four important risks that must be addressed.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Paul Laughlin is the founder of Laughlin Consultancy, which helps companies generate sustainable value from their customer insight. This includes growing their bottom line, improving customer retention and demonstrating to regulators that they treat customers fairly.
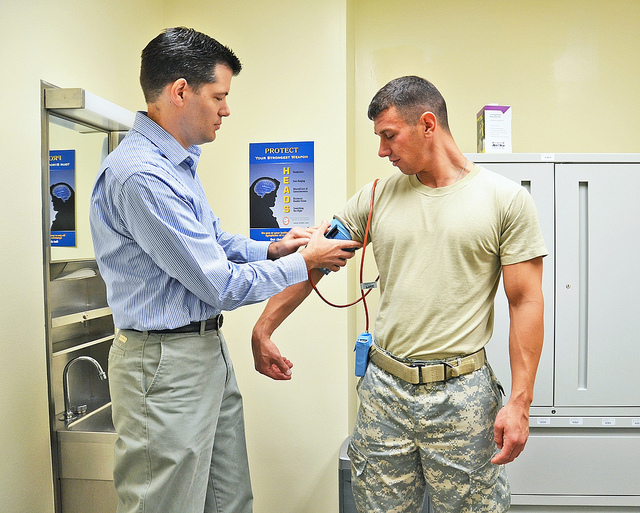
Answer: very rarely. Even leaving aside the public health issues they create, opioids simply aren't very effective at treating pain.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Donald Teater, MD, is responsible for advising National Safety Council advocacy initiatives to reduce deaths and injuries associated with prescription drug overdoses. Teater is a patient advocate who specializes in psychiatric services and opioid dependence treatment.
Telemedicine, Google Glass, wearable monitor, Internet-connected sensors, 3D printing and robotic devices can all improve quality and cut costs.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Kimberly George is a senior vice president, senior healthcare adviser at Sedgwick. She will explore and work to improve Sedgwick’s understanding of how healthcare reform affects its business models and product and service offerings.
In the second article in a series, the author -- himself just 21 -- explains how to start to build relationships with young prospects.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Justin Peters, currently 21 years old, works for an insurance brokerage near St. Louis. He started his career as an intern more than two years ago, with little exposure to the industry and no initial decision to pursue a position in the field after graduation.
If we were ever under the illusion that the rule was an inflexible legal concept, this case should certainly dispel the notion.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Richard (Jake) M. Jacobsmeyer is a partner in the law firm of Shaw, Jacobsmeyer, Crain and Claffey, a statewide workers' compensation defense firm with seven offices in California. A certified specialist in workers' compensation since 1981, he has more than 18 years' experience representing injured workers, employers and insurance carriers before California's Workers' Compensation Appeals Board.
Companies should consider switching to auto-enrollment in retirement plans, because inertia keeps too many from signing up.

Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Matt Page has more than 15 years of experience in financial planning. He specializes in comprehensive, goal-based financial planning, investment management and group retirement plans.
Page graduated with a bachelor of science degree in finance and economics from the University of Oregon. During his career, he has attained certified financial planner (CFP) and chartered retirement plan specialist (CRPS) credentials.