|
April 2026 ITL FOCUS: Underwriting
ITL FOCUS is a monthly initiative featuring topics related to innovation in risk management and insurance.

ITL FOCUS is a monthly initiative featuring topics related to innovation in risk management and insurance.

|
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Insurance Thought Leadership (ITL) delivers engaging, informative articles from our global network of thought leaders and decision makers. Their insights are transforming the insurance and risk management marketplace through knowledge sharing, big ideas on a wide variety of topics, and lessons learned through real-life applications of innovative technology.
We also connect our network of authors and readers in ways that help them uncover opportunities and that lead to innovation and strategic advantage.
A former president of Tesla just published the management "algorithm" that Musk uses at his companies -- and the insurance industry could benefit from parts of it.

Here's a thought experiment for you: What if Elon Musk ran an insurance company?
Just imagine how regulators would react to his brash, visionary ideas wrapped in disdain for tradition and a belief that rules don't apply to him.
But what if you could bottle the good parts of his iconoclasm and leave out the parts that would scare policyholders about the reliability of their insurance carriers? A former president of Tesla just published a book that might allow for that. It describes the five-part "algorithm" that he and Musk used to manage the company during a transformative stretch in the mid-2010s.
I don't think insurers should go full force, a la Musk's "hardcore" mode--you could wind up with an embarrassment like DOGE and never recover--but his algorithm does offer a playbook for radical simplicity and for what I think is the right way to approach automation.
Jon McNeill, author of "The Algorithm: The Hypergrowth Formula That Transformed Tesla, Lululemon, General Motors, and SpaceX," says the method has five steps:
McNeill writes about how Tesla, for instance, questioned China's requirement that it own a piece of any company operating in the country and eventually negotiated a deal that let Tesla own 100% of its Chinese subsidiary. He also writes about deciding that cars didn't need to be assembled out of so many parts, even though they had been since the days of Henry Ford. Instead, Tesla began experimenting with casting bigger and bigger pieces of the car and eventually succeeding, greatly reducing the need for assembly.
For insurers, though, I'm thinking the real benefit would come in more modest ways that track more closely with an anecdote McNeill told in a podcast with the Wall Street Journal. He talked about how much trouble Tesla had designing and manufacturing a part that was supposed to sit between a battery and the chassis. The problem became so important that Musk got personally involved and haunted the factory for weeks. Eventually, Musk and McNeill asked if the part was really necessary, and the battery people told them it had been mandated by the folks responsible for damping noise. When McNeill went to them, he was told that, no, the battery folks had mandated the part to minimize danger in the case of a battery fire. McNeill decided to track down the engineer who had signed the order requiring the part -- and learned he couldn't reach the person because he was a summer intern who no longer was at Tesla.
Insurers already question what they believe to be undue regulation, but I think they could benefit more broadly from asking employees across the business to question everything they're told to do, whether by someone inside the organization or outside it. Even if you just do this as a one- or two-month exercise, I'd bet you'll find you're doing lots of things just because they've always been done that way, not because they deliver any value.
At Tesla, McNeill said in the podcast, he deleted several steps, and Musk asked whether he'd broken the process as a result and received some severe pushback. When McNeill said he hadn't, Musk told him he hadn't gone far enough. He needed to keep pushing until he not only got close to the bone but cut into the bone -- at which point, he should back off and find a sustainable approach.
McNeill said the rule of thumb was to only deliver what the customer directly paid for: the car. Customers didn't pay directly for manuals, for documentation, and so on, so Tesla would spend as little effort as possible in those areas.
Again, I don't think that approach would survive at an insurance company. Cut-until-you-break-something can happen in a manufacturing process, behind the scenes, but it didn't even work at the Department of Government Efficiency (DOGE), which Musk ran in the early days of the second Trump administration. Even with the slash-and-burn ethos of Trump 2.0 a year ago, Musk cut too deeply and caused problems both for those receiving government services and for Trump.
Still, insurers can suffer from a sort of data and process bloat. Given the industry's abundance of caution, it's easy to ask for more questions, to gather more data, and to require another guardrail in the process. Life insurers have shown that it's possible to do the same with less, given the success of fluidless underwriting, and other lines could surely scale back some requirements, too -- becoming more efficient while making customers happier.
I'm combining the last three parts of the Tesla algorithm because, at least for insurers, they all fit under one mandate: "Automate last."
McNeill said Tesla learned the value of these three steps when it was having so much trouble manufacturing the Model 3 that it was running out of cash and was in danger of bankruptcy. The company stopped running its highly automated manufacturing line, set up a big tent outside the factory and started making the cars by hand. Once management figured out the best process, it began speeding up. Only once they saw that they could run the process at speed did they start bringing in the machines that would automate it -- scrapping the entire production line that they'd set up before fully understanding what was needed.
"Automate last" fits with the approach the computer industry has taken for decades: Once a manual process is fully mapped out, it can move into software and then, when you're sure you have everything nailed down, you can hard-wire the work by moving it into the silicon.
That approach makes sense for insurers, too. When you see the possibilities of AI, for instance, you should map out a potential new process, implement it manually, speed it up -- and only then let the machines take over.
There are plenty of things about Musk's approach to business that I wouldn't recommend. For more than a decade now, I've been mocking his annual claims that he'll have millions of Teslas functioning as robotaxis, that he's going to colonize Mars (we won't even land someone on Mars in his lifetime), that he's about to unleash an army of humanoid robots, and so on. Those of us without his massive wealth would lose all credibility overnight if we pushed a similar sort of sci-fi dream. Insurance, as an industry built on trust, can't afford anything close to the wild claims that Musk makes routinely.
But I do think it's worth giving his algorithm serious consideration because it can reduce complexity and lead to effective automation. If nothing else, reading about the bold moves at Tesla might inspire some new thinking and resolve in the insurance industry.
Cheers,
Paul
P.S. "The Algorithm" reminds me of one of my favorite geek jokes:
Q. How do we know that Al Gore actually invented the internet?
A. It runs on Al-Gore-ithms.
The 10 Providers That Matter Most And How They Stack Up

Digital insurance agency platforms are the cornerstone of the insurance ecosystem. With digital first consumers demanding seamless experiences, agencies and carriers need technology that delivers speed, insight, and engagement. Zywave received the highest rank of all vendors in the strategy category, and maximum possible scores in the innovation, vision, and roadmap criteria in this report.
The report provides a comprehensive evaluation of insurance technology platforms, analyzing current offering and strategy. See how Forrester evaluated 10 top platforms, and why Zywave earned the highest score in the strategy category and the highest possible scores in the criteria of vision and innovation.
The Forrester Wave™ report noted:
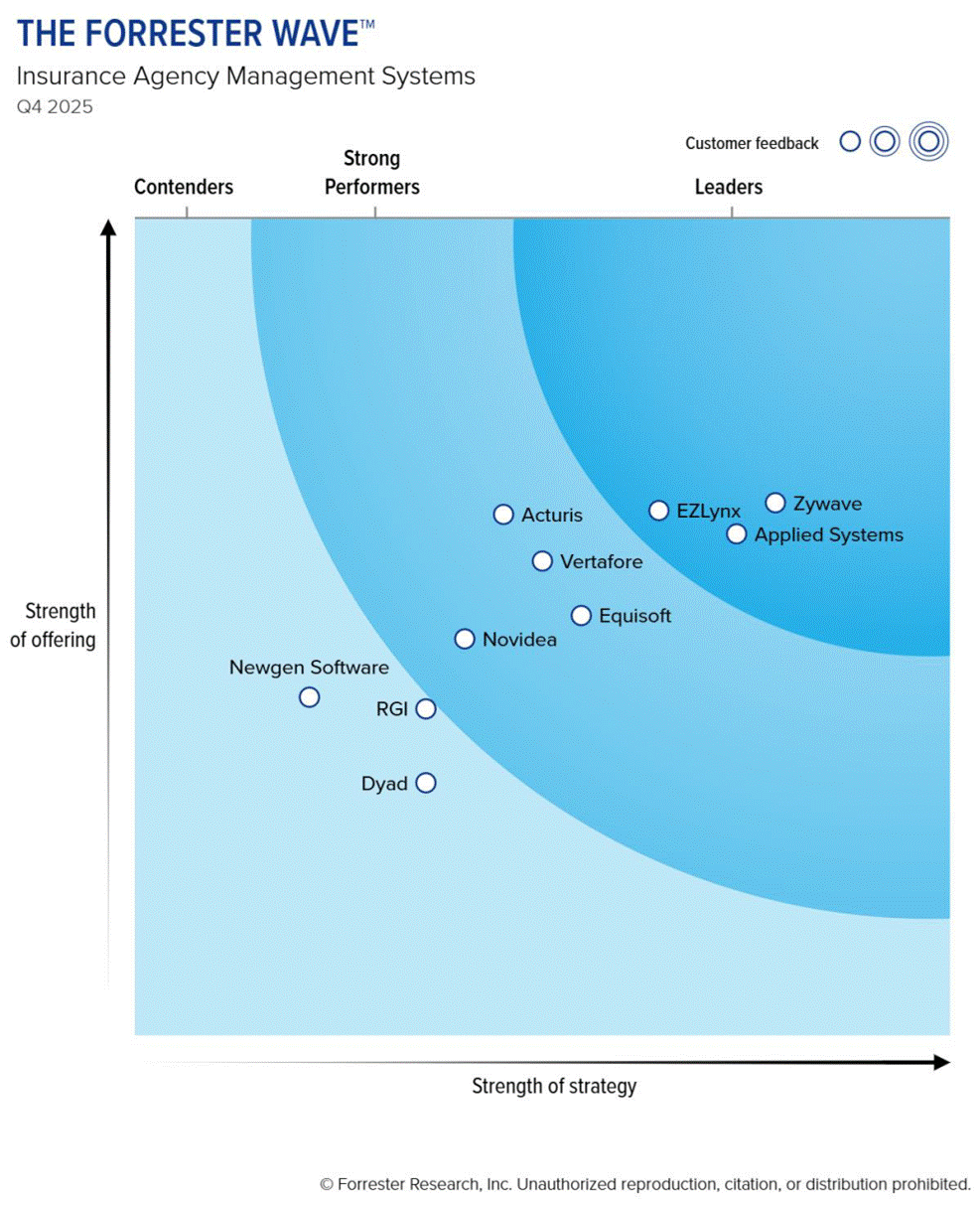
Sponsored by ITL Partner: Zywave
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Zywave delivers AI-powered growth engines for the insurance industry, enabling carriers, MGAs, agencies, and brokers to grow profitably, strengthen risk assessment, enhance client relationships, and streamline operations. Its intelligent, AI-driven platform acts as a performance multiplier for more than 160,000 insurance professionals worldwide, across all major segments. By combining automation, data insights, and best practices, Zywave helps organizations stay competitive and efficient in today’s fast-changing risk environment—empowering them to adapt quickly, scale effectively, and achieve sustainable growth.
For more information, visit zywave.com.
While claims technology has improved for decades, too little has been done to leverage it. It's time to move beyond document storage and into effective decision-making.

The insurance claims industry sits at an inflection point. Medical records are more complex, nuclear verdicts are rising, and the workforce is changing faster than most organizations can adapt. AI promises to help — but most implementations have fallen short. We sat down with Mark Tainton, senior vice president of data solutions at Wisedocs, to talk about what's actually working, what isn't, and why the industry needs to move from document management to true decision intelligence.
The insurance claims industry has been talking about digital transformation for years. What's actually changed in the last 18 to 24 months, and what's still stuck?
Having worked in the insurance industry for over 30 years at the intersection of technology and claims operations, I've certainly seen infrastructure change. But the bigger question now is the operating model that can actually leverage that infrastructure. And the operating model is not so much around storing documents in claims management systems or document management systems—it's about how we take advantage of that data asset. We’re essentially moving from document storage into effective decision-making.
Over the last five years, there has been an acceleration in the technology, in particular with large language models. Technology is not the problem.
It's really about taking advantage of the individual pieces of information in the world of unstructured data. That's the next wave we should be focusing on: How do we operationalize the assets so they’re part of the DNA of insurance processes?
Medical record review is at the heart of so many claims decisions, yet it still appears remarkably manual at most organizations.
I’ve certainly seen large carriers that have introduced AI but haven't introduced the process changes or changed how people can take advantage of the insights as the claim goes through its lifecycle. Carriers are using ineffective decision making approaches that continue to mirror what we saw 10, 15, 20 years ago.
There needs to be a conversation around how adjusters work, especially because of the change in their age demographic. New people coming into the claims industry consume data completely differently. We have to adjust.
You have to also understand the psychosocial aspects of the workforce, where COVID accelerated change. You need to cut across multiple claims at any given time and look for triggers that are prevalent by a treatment provider, or at risk indicators that suggest psychosocial issues—they are top of mind for a lot of claims teams right now.
There's always a tension between speed and defensibility in claims, especially given the high stakes. How do insurers resolve that tension?
Claims are getting more complex, and we've seen a lot of legislation that makes it very clear that if someone's making a decision solely based off AI output with no human in the loop, that's going to be a problem.
When you tie that concern into the expansion of traditional fraud and increases in nuclear verdicts, the defensibility question becomes critical. There needs to be a human in the loop.
Several states are already drawing that line legislatively. California's SB 574 and a growing number of AI governance frameworks now require that AI-assisted decisions in insurance and legal contexts be documented, auditable, and explainable. That is not a future concern; it is a present operating requirement for carriers doing business in those jurisdictions. The organizations that build defensibility infrastructure now will not be scrambling to retrofit it later.
There are a lot of solutions out there these days, but they seem to largely be point solutions—summarization tools, triage tools, document processors, and so forth. What's missing from the point solution approach?
First, they don't fit into the ecosystems of clients and large carriers. They don't work alongside platforms like Guidewire where they can function as a module and help make those decisions effective.
The point solutions also aren’t really end-to-end. They're focusing on a point in time on a particular claim. That produces what I call a silent failure. The AI processes the document and returns a summary, and the claim moves forward. But the anomaly that should have triggered a flag, the treatment pattern that does not match the diagnosis, the billing inconsistency that signals a problem: None of that surface because the tool was never designed to look across the lifecycle. The claim does not fail loudly. It just quietly travels in the wrong direction for months.
Think about first notice of injury as a claim goes through the life cycle, and all of a sudden you get a demand package or a treatment package coming in. What are the decisions you want the adjuster to make?
You need intelligence that cuts across the full lifecycle of the claim in terms of other claims with certain characteristics. And I think that's where point solutions really come up short.
I assume that thinking is why you took a platform approach with WiseShare.
Very much so. We have the sorting and summarization solution that we just renamed WisePrep. It includes WiseChat, where users can save all the insights they generate from a large language model. We've introduced WiseInsights looking at litigation trends, looking at treatment patterns and how they develop, looking across claims that an adjuster who's got a workload of 200 or 300 claims cannot identify on their own. These insights reveal similar characteristics across claims. For example, we looked at one portfolio and identified that a particular treatment provider, over a 12-week program, consistently prescribed a higher and more severe medication at the four-week timeline.
WiseShare is important, too. Far too often, a summarized document gets passed from the adjuster to inside counsel, then to external counsel, and eventually to an IME [independent medical examiner]. A lot of the time, we see slip-ups—documents go missing, misinterpretations occur, different versions of the truth emerge. WiseShare brings everything together into one consolidated environment where all of those entities can actually share, review, and export the claim file.
From a legal defensibility standpoint, that consolidation is not a convenience; it is a chain-of-custody argument. The defense bar needs to see a complete, unbroken record: the medical record chronology, the time series of decisions made, and documented consistency in how AI processed the underlying materials. When a claim ends up in litigation, the question is not just what decision was made; it is whether that decision can be reconstructed, sourced, and defended at deposition. WiseShare is built for that standard.
You have to be able to wrap intelligence around a decision, and that requires a platform.
Decision intelligence needs to be comparative. You have to be able to see the claim you're dealing with in the context of other claims. The intelligence also needs to be sequential. Are we seeing similar patterns starting to develop on other claims in certain jurisdictions? Are we starting to see certain seasonal trends? Are we starting to see different types of treatment coming through? Finally, the intelligence must provide accountability. Is every inference sourced and every decision point documented?
The defense bar needs to see that audit trail. They need to see the medical record chronology, the time series, and the consistency in terms of best practices for how AI actually processes documents and insights for better outcomes. From 2023 to 2024, nuclear verdicts rose 52%. Thermonuclear verdicts are up 81%, and overall verdicts are up 116%.
You need one single environment where you store the materials, one single process that's consistent across an organization.
Bottom line: if you can't show defensibility, you're in a world of trouble.
There's discussion about AI replacing many human workers in the insurance industry. What is your perspective?
There's this notion that AI is going to replace people at the desk. From my perspective, that's totally inaccurate. And I think that mindset sets back adoption.
But here's the inflection point: We're dealing with an aging workforce. Insurers and TPAs are struggling to attract talent. Why? Because some of the tools and technology have not evolved as quickly as in other industries. When you can walk hand in hand with AI and the person at the desk and show them all the benefits, that’s exciting.
If you could change one thing about how the insurance industry is currently approaching AI adoption in claims, what would it be?
For me, it's what I call the evolution framework. AI is a journey, not a one-time event. Far too often, what I've seen is large organizations—mid-tier, tier two, tier three—treating this as basically an implementation. It's almost like they're going in, turning the light switch on and walking out.
I spend quite a bit of time working with clients all the way from inception to asking: Where are we actually going to implement this? What's the impact we're expecting? How does this align with strategic objectives? What are some of the key measurements we want to see in terms of adoption, change, and, ultimately, having the AI start to hit the hard dollars—reduction in litigation, average duration, and things like that.
I'll give you an example. I worked with a large carrier that wanted to implement AI across the entire organization. But they have an aging demographic in certain lines, and getting them to adopt AI would be difficult. They've also captured a lot of information very poorly in their systems—it's very much in their heads.
I said, Let's focus on the younger generation. They’ll adopt AI, and we’ll create a best practice, one that we can use when we bring in new talent. So we built a three-year program focused on them. Ultimately, the program was so successful that the older generation said, We want to be part of that, too.
For me, the next window for anyone embarking on an AI journey is to focus on embedding it upfront—knowing, of course, that the process will evolve over time.
Begin with what we call an EDA—exploratory data analysis—to determine what the baseline is. That way, you can prove that you’re opening and closing claims far more quickly and can see the change quarter over quarter. That data helps sell the journey. We've also done quite a bit of work around what we call data quality programs, where we assess the quality and change behavior at the desk in terms of how people are capturing data—all the way from structured to unstructured and, more importantly, in the adjuster call notes. That program embeds the solution into the fabric of the organization.
I think that's the next wave.
Thanks, Mark.
Sponsored by Wisedocs
Mark Tainton is the SVP of Data Solutions at Wisedocs, bringing over 30 years of AI, data and analytics transformation expertise in insurance and financial services. Having served as Chief Data Officer at multiple leading organizations, Mark understands the critical intersection of medical intelligence, litigation strategy, and claims outcomes. He advises Wisedocs on data and product strategy, go-to-market positioning, and the deployment of AI-powered solutions that address the most pressing challenges facing claims and legal professionals today.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Insurance Thought Leadership (ITL) delivers engaging, informative articles from our global network of thought leaders and decision makers. Their insights are transforming the insurance and risk management marketplace through knowledge sharing, big ideas on a wide variety of topics, and lessons learned through real-life applications of innovative technology.
We also connect our network of authors and readers in ways that help them uncover opportunities and that lead to innovation and strategic advantage.

Wisedocs is an AI-powered claims documentation platform purpose-built for insurance and medical record processing. Trained on over 100 million claim documents, the platform delivers structured, defensible outputs, from summaries to insights, all with expert human oversight. Wisedocs empowers enterprise carriers, government agencies, legal defense teams, and medical experts to improve operational efficiency, reduce administrative burden, and enhance decision accuracy. Visit www.wisedocs.ai to learn more.
It's time to stop simply reacting to plaintiffs' counsel and to become more aggressive through data-driven counter-anchoring.

Brute force has been the corporate response to the normalization of nine-figure payouts—build taller insurance towers. But by 2026, we've reached the breaking point of that strategy. Adding more capacity is no longer a hedge; it's a target. Leaders who continue adhering to a "wait-and-see" strategy will likely hand over their negotiating power to plaintiffs' counsel. It's time to stop reacting and shift to a more aggressive tactic of data-driven litigation counter-anchoring, a tactical maneuver that uses historical benchmarks and hard modeling to ground a case's valuation.
Refusing to name a number isn't a denial of liability; it's a tactical surrender. When we stay silent and treat it as a problem for later, we leave a vacuum that the plaintiff is only too happy to fill. This is the psychology of anchoring: the first number heard becomes the mental hook upon which all subsequent negotiations hang. If the opening bid is a $100 million "lottery ticket," even a successful defense that cuts it in half results in a $50 million disaster.
Counter-anchoring disrupts this by providing a grounded alternative before the plaintiff's number can take root. This isn't a guess; it is a calculated figure backed by historical industry benchmarks and internal safety data. By presenting a credible, data-backed valuation early, we offer juries a "safe harbor."
Most jurors are actually overwhelmed by the emotional volatility of nuclear-risk cases; they want to be fair, but they lack a yardstick. When the defense provides that yardstick—derived from logic rather than emotion—it grants the jury the permission they need to reject an inflated demand without feeling they are dismissing the injury itself.
Counter-anchoring is most effective in "gray area" liability cases—scenarios where the question isn't if the company is responsible, but for how much. In these high-value moments, the goal is to cap the ceiling before it vanishes. By introducing a data-backed valuation early in mediation, you effectively narrow the range between "reasonable" and "astronomical."
However, data is a double-edged sword. The greatest risk in this strategy is the "Cold Corporation" trap. If your counter-anchor looks like a sterile spreadsheet in the face of a human tragedy, you don't just lose the argument; you lose the jury.
There is a razor-thin line between being "grounded in reality" and being "callous to suffering." The math must be the foundation, but the delivery must be human. If the jury perceives your data as a tool to devalue a life rather than a method to find a fair resolution, the anchor will drag your defense to the bottom.
When executed with empathy, speed becomes your primary weapon. By removing the "valuation fog" early in the process, counter-anchoring forces both sides to deal with reality. It strips away the performative inflation of the discovery phase and gets to the heart of the settlement, often shaving months—and millions—off the litigation lifecycle.
In 2026, a spreadsheet is not a strategy. While internal loss runs are necessary, they are rarely sufficient to move a jury. To make an anchor stick, you must look beyond internal data. A jury will instinctively view a company's own historical figures as self-serving; to achieve true "safe harbor" status, your numbers must be validated against industry cohorts. Credibility is built on external benchmarks—proving that your valuation isn't just what you want to pay but what the broader market defines as objective reality.
The most critical hurdle, however, is the communication gap. Raw modeling is the foundation, but the courtroom narrative trumps all. If you cannot translate a complex actuarial model into a story about fairness and community standards, the data will be dismissed as "corporate math." The numbers provide the boundaries, but the narrative provides the "why."
Finally, this strategy demands a collapse of the traditional corporate silo. We are seeing the rise of the general counsel/risk manager nexus. In the past, Risk bought the insurance, and Legal fought the claims. Today, these two must merge their datasets well before a summons is served. By aligning on valuation models during the underwriting phase, the defense is armed and ready on Day 1 to set the anchor before the ink on the complaint is even dry.
Adopting a counter-anchoring strategy does more than win cases; it fundamentally shifts the power dynamic at the renewal table. In the 2026 market, excess underwriters are no longer just looking at loss history—they are scrutinizing a firm's "litigation maturity." When you can demonstrate a repeatable, data-backed method for suppressing social inflation, you move from being a commodity risk to a "preferred risk."
The conversation with underwriters changes the moment you move beyond passive risk transfer. Instead of simply presenting a tower of limits, you are presenting a proactive defense framework. Underwriters are tired of "blank check" litigation; showing them that you have the tools to anchor damages early provides them with something they value more than anything: predictability. By proving you can cap the ceiling of a potential nuclear verdict, you provide the actuarial certainty that justifies lower attachments or more competitive pricing.
The ultimate result is a stronger strategic partnership with your carrier. You aren't just buying paper to cover a potential disaster; you are demonstrating a sophisticated operational control that protects the carrier's capital as much as your own balance sheet. In an era of escalating awards, the companies that thrive will be those that prove they aren't just insured against the storm—they have the data to ground the lightning.
The era of "buying our way out" of litigation risk is over. In a 2026 landscape where $100 million is the new baseline for a nuclear verdict, silence on damages is a luxury no risk team can afford. By embracing data-driven counter-anchoring, general counsels and risk managers can reclaim the narrative, providing juries and mediators with a logical "safe harbor" before the emotional tide takes over.
Success now requires a fusion of math and empathy—a strategy where the data is the foundation, but the story is the house. Ultimately, those who anchor early won't just lower their payouts; they will redefine what it means to be a resilient, data-forward organization in an age of outsized expectations.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Jonathan Selby is managing director at Founder Shield.
Banks lost customers' trust one automated interaction at a time. Insurers are making the same mistakes.

In 1979, Gallup asked Americans how much confidence they had in banks. Sixty percent said a great deal or quite a lot. Banks ranked second out of nine institutions — behind only the church.
Today that number is 26%.
The collapse didn't happen because of one crisis or one bad actor. It happened over 40-plus years, one automated interaction at a time. ATMs that replaced tellers. Interactive voice response systems that replaced those ATMs. Digital channels that replaced the IVR. And now AI-driven decisions replacing the digital channel that replaced the thing that replaced the person who used to know your name.
Each wave came with a business case. And each wave, when it touched the moments that actually matter to customers — a confusing charge, a decision that needed explanation, the thing that went wrong at the worst possible time — quietly withdrew a small deposit from an account that doesn't show up on any balance sheet.
That account is trust. And trust, it turns out, is an organizational capability problem — not a sentiment problem.
Here's what I observed working inside a global bank during those automation waves: the technology worked. The process was faster. The costs came down. And customers were fine — until they weren't.
When something went wrong, people didn't want a faster process. They wanted a person who understood the situation, had the authority to act on it, and demonstrated that the institution they'd trusted actually cared what happened to them. What they got, too often, was a system designed for the average case, handling something that wasn't average at all.
What struck me wasn't the technology failure. It was the organizational failure underneath it. The leaders driving automation were making efficiency decisions. Nobody was accountable for the capability question: Does this organization know how to rebuild trust when the automated system fails a real person? The answer, in most cases, was no — because that capability had never been built. It had been assumed.
That pattern — confusing an efficiency decision for a capability decision and discovering the difference too late — is what eroded four decades of public confidence in banking. And it's the pattern insurers are now repeating.
Insurers are making the same bet banks made, in the same places banks made it.
Claims. Denials. Coverage decisions. Underwriting. These are not commodity interactions. They are, almost by definition, the moments when a policyholder is most vulnerable — a damaged home, a health crisis, a business interruption, a death. They are the moments that test whether the relationship the insurer sold is real.
The industry is automating them anyway. With AI systems that make faster decisions, with chatbots that handle first contact, with models that assess claims before a human ever sees them. The business case is real. The efficiency gains are real. The risk is also real — and it is being systematically underestimated.
Here's what gets missed in most of these conversations: The risk isn't primarily in the technology. It's in the organizational capability gaps the technology exposes. Does this organization have the judgment infrastructure to know when a claim needs a human? Does it have the change leadership — not change management, but genuine leadership capability — to ensure that the people still in the room when it matters are empowered to act? Can it tell the difference between a process that's working and a relationship that's quietly eroding?
Most organizations can't answer yes to all three. Not yet.
Here is the part the business case doesn't model: what automation does to the agents and claims professionals who remain.
When an organization systematically automates the high-stakes moments, it doesn't just remove humans from those interactions. It degrades the humans who stay. Authority gets stripped. Judgment gets overridden. The agent or adjuster who once had the latitude to assess a situation and act on it becomes an escalation path for complaints the system couldn't handle — without the context, the tools, or the organizational backing to actually resolve them.
This matters because the agent is still the face of the insurer when the policyholder calls. The claims handler is still the voice on the other end when the denial needs explaining.
The data on this dynamic in financial services is stark. An Eagle Hill Consulting survey of more than 500 U.S. financial services employees found that 62% say their organizations have prioritized improving customer over employee experience — yet those same employees report that their own work experience directly affects their ability to serve clients. Dissatisfied employees are more than three times as likely to report that their negative work feelings reduce their willingness to help others.
Deloitte's research adds another dimension: When AI tools are introduced without careful design and change leadership, employees perceive their organizations as nearly two times less empathetic and human. That dynamic doesn't stay inside the organization. It travels. Policyholders feel it.
For insurers that rely on independent agents — professionals whose loyalty is earned, not owned — the stakes are even higher. Think of independent agents as the community bankers of insurance: For decades, they've translated corporate rules into human terms, sitting across the table from policyholders at the moments that matter most. J.D. Power's independent agent satisfaction research consistently finds that scores are dramatically higher — by hundreds of points — when carriers make agents easier to work with: faster quotes, transparent claims status, access to a human on complex cases. When AI becomes a black box agents can't explain to a policyholder, that advantage reverses. An agent who can't get a straight answer on a claim denial, or can't reach a human on an exception, doesn't complain to the carrier. They quietly shift their next piece of business elsewhere. The trust problem isn't just with policyholders. It runs through the entire distribution chain.
What makes this dynamic particularly dangerous is that trust erosion is invisible on a quarterly basis.
The banking sector learned this the hard way in early 2023. When Silicon Valley Bank failed, uninsured deposits left the broader banking system at the fastest rate recorded since the FDIC began tracking data in 1984 — an 8.2% quarterly decline, industry-wide, in a single quarter. The FDIC noted that SVB's deposits were "remarkably quick to run" precisely because they were concentrated among depositors whose trust, once shaken, had no friction to slow it.
Insurers don't face bank runs. But they face their own version: policy non-renewals, lapse rates, coverage migration, claims disputes that become regulatory attention, and the slow erosion of the trusted advisor position that has historically made insurance a relationship business.
The erosion rarely announces itself. It accumulates in policyholder satisfaction scores that drift, in agent feedback that doesn't make it up the chain, in claims handling data that gets read as operational variance rather than relationship signal. By the time it's visible on the balance sheet, the capability gap that caused it has been open for years.
The research on AI deployment in financial services confirms what the banking experience suggests. McKinsey finds that AI high performers are more than 1.5 times as likely to have changed their standard operating procedures and talent practices — not just deployed tools. MIT CISR shows that firms stuck in the pilot stage financially underperform their industries, while those that have embedded AI into their operating models significantly outperform.
What those numbers describe, underneath the data, is an organizational capability gap. The high performers aren't distinguished by better technology. They're distinguished by having built the mindsets, the skillsets, and the operating conditions — the governance, the decision rights, the human judgment infrastructure — that allow them to absorb what the technology makes possible without losing what made them trustworthy.
That's the real lesson from banking. The institutions that automated their way into a trust deficit weren't led by people who didn't care about customers. They were led by people who treated trust as a communications challenge rather than a capability one. They managed it. They didn't build it.
Insurers now face a choice that banks didn't get to make deliberately. Insurers can design AI deployments that preserve human judgment at the moments that matter most. They can build the change leadership and workforce capability that determines whether AI enhances the relationship or quietly erodes it. They can treat trust not as a sentiment to be managed after the fact but as an organizational capability to be built before the moment of truth arrives.
Or they can assume their situation is different from banking.
Banks assumed that, too.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Amy Radin is a strategic advisor, keynote speaker, and Columbia University lecturer focused on why transformation succeeds or stalls in large, complex organizations.
Drawing on senior leadership roles at Citi, American Express, and AXA, including one of the world’s first corporate chief innovation officer roles, she helps leaders build the capabilities required to absorb, scale, and sustain change.
The just-concluded NCAA Wrestling Championships showcased the sort of thorough competitive advantage that can come from early success with AI.

As the Penn State wrestling team won yet another Division 1 title over the weekend--its 13th of the past 16 awarded--and did so in overwhelming fashion, I realized there is a deeper competitive advantage at play than exists even in other sports.
College wrestling dominance requires a layer that goes beyond the normal advantages that come from having a great coach and a roster of superb college athletes. Penn State-level dominance in wrestling requires an additional, self-reinforcing factor--of the sort I think can come from early success with AI, as it builds and builds and builds on itself.
I'll explain.
To understand that self-reinforcing factor, you need to look at the Penn State coach and at the coach whose record of 15 NCAA wrestling titles in 21 seasons Penn State is now approaching.
The Penn State coach is Cael Sanderson, arguably the best college wrestler ever. He was undefeated in college, winning 159 matches, and won four NCAA individual titles. He also won a gold medal at the 2004 Olympics.
The man he's chasing, Dan Gable, who coached the University of Iowa from 1976 through 1997, ranks even higher in the wrestling pantheon. He not only won two NCAA individual titles (in an era when freshmen weren't allowed in the tournament) but took the gold medal at the 1971 world championships and at the 1972 Olympics. In those tournaments, Gable won each of his six matches in those tournaments without giving up a point--a preposterous achievement given how scoring works in international wrestling.
Sanderson's and Gable's credentials are so impressive that they naturally attracted top recruits -- and started to build that self-reinforcing layer.
Wrestling differs from most college sports because the very best tend to pursue international careers after graduating but don't have any affiliation akin to what other athletes take on in professional leagues. Post-college wrestlers need a home. They need a wrestling room. And the best go to the best room, making it even better... and on and on we go.
Penn State has easily the best roster of collegiate talent at the moment -- six wrestlers made it to the NCAA finals among the 10 weight classes last weekend, tying the record, and four won titles. And Penn State has even better talent among the international wrestlers, who bring with them scores of NCAA titles and medals from world championships and the Olympics. In the finals of the 190-pound weight class at the U.S. trials for the 2024 Olympics, two wrestlers from that room went up against each other and had an epic battle -- which qualified as just another day in the life of Penn State wrestling.
The insurance industry should, I think, draw a lesson because AI can create a flywheel effect similar to what's happening at Penn State and what happened under Dan Gable at Iowa in the '80s and '90s.
Adopting AI won't happen overnight. Using it is an unnatural act for many people, especially older ones, so you need to find ways to get people to start to get comfortable with it. You need to produce successes that you can use to evangelize about AI. You need to create rock stars that, while not at the level of a Sanderson or Gable, can attract talented people who want to take on more ambitious projects. You need to keep testing and feeling your way toward more aspirational business models, going beyond efficiencies to, perhaps, embedding insurance in other companies' sales processes or developing services that predict and prevent losses before they can occur.
In fact, early successes with AI can generate savings that you can pump into more future projects, so you just keep accelerating.
(I realize I made more or less this point about a flywheel in last week's commentary on Lemonade, but I think it's so important that it's worth reinforcing, and college wrestling turns out to be even a better example than Lemonade.)
No competitive advantage lasts forever. Gable retired at age 48 -- coaches often mix it up with their wrestlers, and even an all-time great eventually wears down. The Iowa program, while still strong, has drifted in the decades since. Sanderson is now 46, and maybe he'll tire out one of these days, too. Meanwhile, David Taylor, a just-retired big name, has set up camp at Oklahoma State, which had four wrestlers make the NCAA finals. Three won. All four are freshman. So another cauldron of a wrestling room may be taking shape.
But I'll bet any insurer would be happy with an advantage on AI of the sort that Sanderson has produced at Penn State and that Gable developed at Iowa before him.
Cheers,
Paul
Insurance quietly underpins America's 35 million small businesses -- a noble purpose that we can serve even better.

Insurance is often portrayed as the bad guy. Or at best, it isn't talked about at all. Business owners want to get a quote, check the box, and move on with their lives. Insurance is background noise, something you deal with because you have to. You don't open a bakery to buy insurance; you do it because you love baking.
However, invisibility is exactly what makes insurance so easy to take for granted. While no one is thinking about it, insurance is quietly doing something remarkable: holding up the entire small business economy.
The United States is home to 35 million small businesses. They're the coffee shop where they know your name. The contractor who rebuilt your deck. The nail salon run by a first-generation immigrant who left everything behind for a shot at something better. They are the economic and social fabric of every community in this country, and they represent something fundamental about what America is — a place where anyone, regardless of where they come from, can build a rewarding life through their own effort and ingenuity. Behind every one of those businesses is someone who took an enormous personal risk. They put up their savings, left a comfortable job, took out a loan, or bet on themselves. What often goes unrecognized is the role insurance plays in making that bet possible.
That's why insurance is the oil that powers the engine of small businesses, the foundation of the U.S. economy. Put another way, insurance is the foundation on which American economic exceptionalism sits.
Consider how much of the small business ecosystem depends on insurance. A coffee shop can't sign a lease without liability coverage. A contractor can't bid on commercial jobs without workers' comp. A nail salon can't stock inventory without property insurance. The banks that approve loans, the landlords that sign leases, and the partners that sign contracts rely on the protection insurance provides to do business at scale.
At its core, insurance is an extraordinarily powerful risk transfer and aggregation system. It gives entrepreneurs the confidence to invest capital, hire employees, and expand. It gives their partners and lenders the confidence to bet on them. This is the kind of infrastructure that makes large-scale entrepreneurship possible, and America has built one of the most sophisticated versions of it in the world.
The downstream effects are profound. I've personally seen small businesses earn enough to send the first member of their family to college. Entrepreneurs across the country have turned a modest storefront into a multi-location operation, creating jobs and employing dozens of people.
It also helps create the next generation of doctors, lawyers, founders, and the next generation of small business owners. Insurance is the safety net that keeps that cycle going.
And despite this, the insurance industry has been slow to modernize. Too many business owners still associate the process with reams of paperwork, phone calls, and fax machines. Too often it takes weeks to get a quote, premiums are priced with a one-size-fits-all model, and the process feels opaque and frustrating.
Making insurance faster to obtain, easier to understand, and more precisely priced has real economic consequences. Every friction point we remove is a barrier lifted for the next entrepreneur. Every small business we protect is a job creator we keep in the game. Every risk we underwrite well is capital freed up to flow toward the next great idea.
Innovating in insurance is exciting because it involves genuinely complex, interesting problems, especially now, as advances in AI and technology give us the tools to finally revolutionize a legacy and yet vital industry.
But what gets me up in the morning is simpler than that. Any time I step into a restaurant or a small shop, I know that while the owners' hard work is what makes their business go, insurance helps give them the confidence to start.
Thirty-five million businesses depend on this industry today. Millions more that haven't started yet will depend on us to make it better. That's a purpose worth celebrating.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Graham Topol is co-founder and co-chief executive officer of MGT Insurance, a vertical AI neo-insurer modernizing commercial P&C insurance for businesses and their agents.
Prior to MGT, Topol worked at FTV Capital, a $6.2 billion fund, focusing on high-growth technology companies in insurtech, financial services, and payments. He also worked at Newfront Insurance, a tech-enabled insurance brokerage valued at over $2 billion, and at Morgan Stanley as a principal M&A analyst and on the staff of the COO.
He earned an AB in economics cum laude from Harvard and an MBA from Stanford GSB.
Deceased policyholders' digital accounts remain accessible to fraudsters but locked to legitimate beneficiaries, creating costly exposure for life insurers.

Policyholders are dying with dozens of open digital accounts, no record of what they own, and no plan for what happens to any of it. When that happens, a fraud window opens. That gap has a cost, and insurers are absorbing it. Life insurance is where the stakes concentrate and the exposure is most acute.
Sandra filed the life insurance claim four days after her husband's death. She had everything she was supposed to have: the policy number, the death certificate, executor authority. Her insurer had 17 unverifiable digital accounts, a death record that hadn't reached the broker databases yet, and a fraud window that had been open since the obituary ran.
That's the default condition for life insurance claims today.
Policyholders maintain dozens of active digital accounts - financial, medical, cloud storage, subscriptions, social media. Many hold documentation directly relevant to estate and insurance administration. Death doesn't close those accounts; it severs access to them.
Only 36% of Americans use password managers, meaning most policyholders leave no systematic record of what they own digitally or how to reach it. Most major platforms offer some form of legacy contact or digital will feature, but adoption remains low. Death leaves a scattered, largely inaccessible digital estate, one that intersects directly with claims management processes.
This is where the exposure becomes the insurer's problem, and that immediate exposure is fraud. After a death, a gap opens between when the death certificate is issued and when that record propagates to the commercial databases that underpin identity verification. During that window, the deceased's digital accounts remain accessible to anyone who can answer a few security questions, questions drawn from the same broker records that haven't been updated yet.
Thieves target recently deceased identities, while life insurers absorb the cost - fraudulent claims, delayed payouts to legitimate beneficiaries, reputational harm when carriers pay bad actors.
There's a legal dimension too. Most platform terms of service were not written with estate law in mind. Even where the Revised Uniform Fiduciary Access to Digital Assets Act (RUFADAA) gives executors legal access to digital accounts, platforms often don't honor it in practice. The beneficiary has a legal right that the platform won't act on. The adjuster has no clean path forward.
Health insurance and workers' compensation face the same fragmentation - medical records, employer portals, and benefit accounts scattered across systems that don't communicate. But life insurance sits at the sharp end of the problem, where the industry's exposure is most acute.
The infrastructure for verifying identity after death has a gap built into it. Deceased individuals' records persist in commercial data broker databases indefinitely, with no real-time connection to official death records. Verification systems that rely on those databases can't distinguish between a living person and a recently deceased one. The fraud window is a consequence of infrastructure that was never designed to handle life transitions.
Sandra's experience perfectly illustrates both sides of that gap. Sandra couldn't get to her husband's financial accounts. Platforms that held documentation she needed for the claim locked her out despite her legal authority as executor. While she was fighting for access, the fraud window that had opened at his death was available to anyone with enough of his personal history to answer a few questions. The accounts she couldn't reach to support her claim were simultaneously drainable by strangers.
Voice cloning and deepfake technology now allow a bad actor to reconstruct a deceased person's voice or likeness from publicly available material, and use it to defeat authentication systems that were never designed with post-death scenarios in mind. As a result, the cost of perpetrating this type of fraud is falling and the risk is rising.
No standard consent or identity framework currently governs the use of a deceased person's biometric data. No enforceable mechanism exists for people to specify how their likeness can be used after death, and insurers have no protection against the claims that follow.
Those who use password managers are ahead of their peers, but individual preparation has a ceiling. Even the most organized policyholder can't force their bank, their cloud provider, and their insurer to exchange data in a standardized way after their death. That requires infrastructure that doesn't yet exist.
The question is: Who shapes that infrastructure? And will the sectors with the most to lose have a seat at the table when the standards are written?
The Death and the Digital Estate (DADE) Community Group at the OpenID Foundation, which I co-chair, recently published a white paper and a planning guide laying out the problem and recommendations for addressing it. Developing interoperable standards for the full lifecycle of digital estate management will require expertise from every affected sector; the insurance industry's knowledge of fraud vectors, claims complexity, and regulatory exposure is specifically what's missing from this conversation.
The groundwork for those standards is being laid now. The sectors that engage early will shape the agenda before the formal process begins. If your organization has a stake in how they get built - and insurers clearly do - the DADE Community Group welcomes participation.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Eve Maler is the founder and president of Venn Factory and co-chair of the Death and the Digital Estate (DADE) Community Group at the OpenID Foundation.
She led identity innovation at Sun Microsystems and ForgeRock, serving as ForgeRock's CTO through Series E, IPO, and acquisition.
Auto dealerships confront escalating risks from cyberattacks to theft rings, demanding comprehensive coverage and mitigation strategies.

Automobiles are becoming increasingly sophisticated and complex, as are the related risks for auto dealers.
For example, in February, 12.5 million accounts with CarGurus were compromised in a cyberbreach that involved the names, email and physical addresses, phone numbers and more of countless customers. CarGurus, a multinational online marketplace that connects car buyers with thousands of dealerships, is facing a bevy of lawsuits over the incident.
Cybercriminals target the auto dealer space because it is fertile ground to harvest the sensitive data collected during the car-buying process, including employment data, bank account information and Social Security numbers. Cyberattacks are now among the top five risks facing dealerships as well as a factor insurance agents and brokers must now consider when advising their dealership clients.
And while all things cyber-related continue to grab both headlines and the attention of consumers, these digital crimes are hardly the only threats driving dealership and car lot-related losses. From old-school auto theft—a risk since Ford's first Model T rolled off the assembly line—to parking lot mishaps, some of these risks are as old as the auto industry itself. However, with the rise of inflation, supply chain challenges and rising costs of litigation, the frequency and severity of these risks, and others, can affect showrooms everywhere that have not prioritized appropriate risk mitigation. As the safety counsel to many business owners, insurance agents and brokers are uniquely positioned to prepare insureds and help manage these threats. This process starts by understanding the complex risks that threaten car lot dealers.
Cyberattacks are far from the only area of concern for auto dealers. Working with an experienced agent or broker, business leaders can not only factor in a range of real-world risks for the industry, but also the severity and frequency of those risks based on their location, inventory types and other factors. Some of these categories might include:
Weather-related claims. Most car lots are exposed to the elements, including hail, storms, winds, heavy rains, snow, ice and flooding and, depending on their location, wildfires. With the increasing frequency of extreme weather and the catastrophic impact of a single-but-severe event, ensuring a dealership's policy factors in weather risks is a critical tool to mitigate high-value inventory losses and lost income from business interruption.
For example, a dealership in Texas suffered a huge financial loss because of a severe hailstorm. To prevent this loss, the business owner could have taken steps including regular monitoring of weather news, installation of a hail netting system and an emergency vehicle relocation plan, all of which would be within the consideration set of an experienced insurance agent specializing in the auto sector.
Organized theft. There has been a rise in vehicle theft, often by organized rings using sophisticated tools like key fob cloning. Installation of a key management system and implementing internal key audit log controls can formalize the process of knowing who takes a key and when, and when it is placed back in the cabinet.
Dealership employees should be educated about the importance of the formalized key check-in/check-out process. We know of a dealership that recently experienced this type of loss when a group of criminals acted as buyers and distracted staff to access vehicles' on-board diagnostics (OBD) ports to program duplicate keys. They returned later and drove off with multiple high-end sport utility vehicles. These risks could have been mitigated through proper employee training where strict supervision is required during test drives, installing OBD port locks and disabling on-boarding capabilities after hours.
As dealers look to better protect themselves, there are many types of coverage that are vital to protecting their businesses. Agents and brokers should offer a comprehensive auto dealer's insurance policy, often including property damage and bodily injury coverage, garage keepers, damage to garage-owned autos and more.
Optional, but often beneficial coverage could also include defective product and faulty work, also known as broadened garage liability coverage, to protect the auto repair side of many auto dealership businesses that might be involved in damage to a customer's vehicle. Dealership owners can also layer in an additional policy to cover the amount of the actual loss of a customer's vehicle, regardless of the dollar limit.
Ensuring the business has the appropriate cyber liability coverage to protect against ransomware and other cyber breaches is now an imperative. In one instance, a phishing email led to a ransomware attack on a dealership that threatened the exposure of confidential dealership customer data. The public release of these sensitive data types can result in extraordinary legal liability as well as bet-the-business-type reputational risks for dealerships. We cannot emphasize enough the need for regular employee education and training on phishing scheme techniques to ensure dealership employees are alert and more likely to spot a threat before the business is compromised.
Finally, agents and brokers have a responsibility to explore and be aware of where and how insureds are using multi-factor authentication on all computer systems and devices to provide increased security of critical data. Understanding where customer data is stored, who has access as well as limiting that access, and the nature of the business' security procedures to protect that data from bad actors must be the new normal of insurance agents to be able to advise clients appropriately.
As the auto industry and technology continue to evolve in their complexity and sophistication, so too will the threats facing auto dealerships. With Bluetooth key-tracking, geofencing devices and real-time telematics, technology tools are continually entering the market to address rising threats. Other resources include AI-powered lot surveillance systems, digital lot movement apps, mobile check-in service for vehicles as well as deploying drones to assist in real-time monitoring of large lot inventories. As threats for auto dealerships grow and evolve, the technology resources to combat them promise to help business owners keep pace.
Insurance agents specializing in fleet insurance owe it to their insureds to keep pace with both the growing risk categories as well as the emerging technologies being employed to mitigate them. That awareness will allow agents to best advise their auto dealership clients as well as help reduce the frequency and severity of related claims across a range of risk categories.
With experienced and knowledgeable advisors, along with a suite of appropriate technology tools available to them, auto dealers can feel confident they remain in the driver's seat of protecting their businesses and mitigating their risks.
Agents should encourage dealerships to think beyond just buying insurance and focus on building good habits into their daily operations. Simple steps like verifying a driver's license before every test drive, keeping strict control over keys, and reconciling inventory at the end of each day can prevent major losses. Service teams should be trained not only on repairs but also on documenting their work and double-checking vehicles before they're returned to customers, especially with today's advanced technology and EV systems.
From a security standpoint, strong lighting, quality camera systems, secure key storage, and clear after-hours procedures go a long way. And because dealerships handle sensitive financial information, regular cyber training and basic safeguards like multi-factor authentication are just as important as physical security. In many cases, it is consistent processes and not expensive upgrades that make the biggest difference in preventing claims.
Get Involved
Our authors are what set Insurance Thought Leadership apart.
|
Partner with us
We’d love to talk to you about how we can improve your marketing ROI.
|

Rajni Kapur is CEO of All Solutions Insurance, one of the largest independently owned insurance agencies in California.